Editor’s note: This series will focus on the difficulties faced by the medical fraternity at COVID-19 hospitals, their duty hours, access to protective gear, facilities they get during quarantine, how are their families coping with this new reality across different states in the country. This is the fourth part of the series.
***
Locked up inside a hotel room, Doctor A spends the hours away from the hospital counting minutes in silence, until it’s time to go back to one of the foremost coronavirus war-rooms of Kolkata — the MR Bangur Hospital, declared a COVID-19 centre earlier this month. Speaking on condition of anonymity, the doctor, a first-year resident at the hospital, sounds exhausted, almost resigned over the phone. “The situation is pretty grim, you know. How much can you fight the system and the government?” Doctor A asks. Despite having a home in the city, the physician has been staying at the accommodation assigned by the hospital after being put on isolation ward duty about a fortnight ago. Food, however, isn’t available at the facility and has to be ordered online. In order to escape thoughts of death and depression, Doctor A resorts to Tiktok-ing with colleagues. “What else do we have? It’s incredibly depressing. We weren’t even given time to prepare for this crisis and the news that the hospital will be turned into a COVID-19 centre was just suddenly announced.” After completing six and 12-hour-long shifts thrice a week at coronavirus isolation wards, the doctor goes back to handling emergency labour cases, or “COVID pregnancies”, without ‘quarantine leaves’ like some of the doctor’s peers at other city hospitals have been granted. “Even though we should ideally be getting seven days off after working at the COVID wards, we are being asked to report to work. And so we are. MR Bangur, at the end of the day, is not a medical college, it’s a district hospital without the necessary infrastructure to deal with a crisis of this scale,” Doctor A tells me. As circumstances changed overnight, hospital staff were left in the lurch without proper training in how to deal with the disease, or even don and dispose of a PPE (Personal Protective Equipment) kit. “We understand that it was an emergency, but we don’t even have the basic training to deal with COVID-19 patients. We started working with doctors and trainees from other medical colleges and figured things out eventually. At least the ones working on the frontlines should be trained in general medicine, chest medicine, and anesthesiology,” Doctor A points out. They aren’t afraid to work, the physician says, but they need to be better equipped to perform their duties, and not just be asked to hand out death certificates at isolation wards like “puppets”. “Patients are dying in front of our eyes, and we can barely do anything about it.” [caption id=“attachment_8302291” align=“alignnone” width=“825”]  A photo of MR Bangur Hospital, Kolkata, taken before the lockdown. Via Facebook.[/caption] However, Dr Monica Saha, another junior resident doctor at the same hospital, seems to be enjoying the challenge posed by the unprecedented medical crisis. For her, it’s an opportunity to rise to the occasion and contribute to society significantly. “Honestly, I wanted to be posted at COVID-19 wards to save lives. PPEs are all in place, so there’s very little to be afraid of for us at the moment,” she tells me while being quarantined at a doctor’s quarter inside the hospital campus. Hailing from a doctors’ family, — with her father Dr Makhan Lal Saha heading the surgery department at IPGMER and SSKM Hospital, Kolkata (a coronavirus testing centre) — Saha chooses to be optimistic, showing faith in the government’s efforts. “I think the situation will be even better-handled once rapid test kits arrive, which should happen in a couple of days. That way, we’ll be able to screen out patients right at the beginning without running the risk of exposing more healthcare workers and patients to the virus,” she says. On 21 April, a day after Bengal received its first batch of said kits manufactured in China, the Indian Council of Medical Research (ICMR) advised states to stop using them following complaints of faulty equipment. Click here to read the complete series Saha’s father, along with friends and family, stepped up and pooled in money to donate face shields to MR Bangur Hospital, which have now been distributed to 175 healthcare workers at the facility. The gears are made of fibreglass used in helmet visors and cover one’s entire face from forehead to chin. “It’s an additional layer of protection since the disease spreads through droplets,” Monica Saha says. The situation, however, is far from similar only 23 kilometres away, at the College of Medicine and Sagore Dutta Hospital in the North 24 Parganas district. [caption id=“attachment_8302301” align=“alignnone” width=“825”] 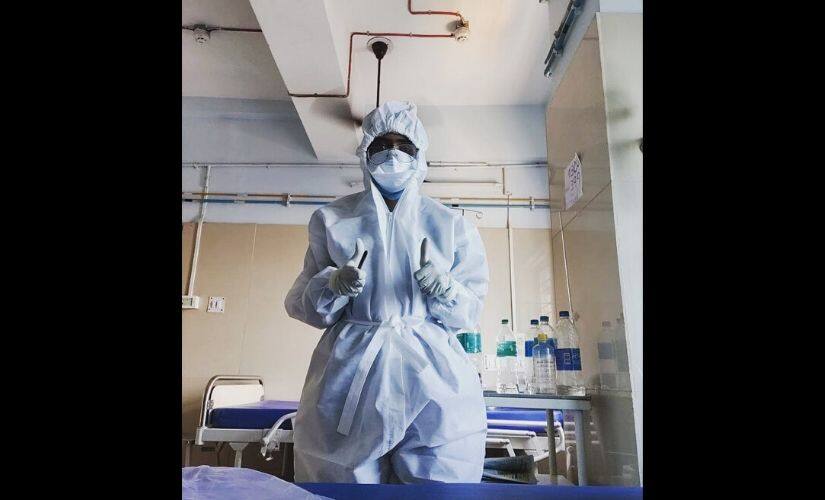 Dr Monica Saha wearing a PPE while on duty at MR Bangur Hospital, Kolkata. Photo courtesy: Monica Saha[/caption] Speaking to us on condition of anonymity, a medical staff working at a COVID-19 isolation ward in Sagore Dutta Hospital — who shall be referred to as Zion hereon — mentions how the protective equipment provided to cleaners at their institute might not be enough. “They’re wearing surgical scrubs underneath raincoats , with N95 masks, face shields and black rubber boots provided to them by the hospital,” Zion says. Primarily being run by a group of 28 interns and a handful of supervising house staff, the isolation wards at the facility have a meagre capacity of eight. “A couple of days back, we found out that one of the patients who was admitted here as a suspect had tested positive. The problem at this facility is a severe lack of manpower. We don’t even know if the suspected patients who are being prescribed tests are actually getting tested or not. If the doctors manage to take patients’ contact details, they’re having to call them personally and find out what happened. Even if anyone tests positive, the test centres aren’t alerting us. The doctors here are having to seek out that information personally,” Zion says. This information is then used to contact-trace every healthcare worker who’d interacted with the suspect on the day of his/her visit, following which, they’re asked to stay under observation in quarantine for seven days, and not for the widely advised period of 14 days. “In general, former day scholars at the hospital who are now interns are having to return home after performing their duties at the isolation wards every day. It’s only when any of them comes in direct contact with a confirmed positive case that they’re offered accommodation at Apex Lodge opposite the college building. They’re asked to observe themselves for seven days to see if they develop symptoms. If not, they’re asked to resume duty from the eighth day,” Zion informs. This system, however, is purely contingent upon attending doctors making a note of the patient’s contact details, failing which they are left in the dark about possible risks of infection. According to the guidelines on the ‘rational use of Personal Protective Equipment’ published by the Ministry of Health and Family Welfare, personnel with thermal guns stationed at the entrances of various facilities fall under the ‘low risk’ category of exposure and are advised to only use triple-layer medical masks and gloves. But Zion has doubts about its efficacy, citing the rising number of cases of healthcare workers testing positive for the coronavirus despite following official protocol. “Our group D staff do not have enough protection. Isn’t this complete exploitation of the lesser privileged classes who are literally putting their lives on the line for meagre pay, just because they don’t have the privilege of sitting at home?” Zion asks, echoing the thoughts of a nurse — who wished to remain anonymous and shall be referred to as Nurse W — working at a COVID-19 isolation ward in MR Bangur Hospital. [caption id=“attachment_8302311” align=“alignnone” width=“825”]  College of Medicine and Sagore Dutta Hospital, Kolkata. Via Facebook.[/caption] Being the only child of parents who live in the city’s suburbs, the nurse wonders what the family must be going through, as the pandemic continues to hold the world hostage in their homes, especially endangering the lives of frontline workers like their child. “They don’t have an option but to accept it as fate,” Nurse W’s voice trails off. They were fearful initially; now, they’re simply numb. “It is what it is, you know? I can’t stop working, even though I am not quite sure about how protected I am wearing the PPEs given to us,” Nurse W says, adding that the protective equipment given to them at MR Bangur doesn’t seem to be made of the same material as the ones being recommended on the internet. “It feels like it’s made of some woven material — very thick on the skin. I don’t know what they are giving at Beliaghata ID, but at least in Bangur, the fabric doesn’t feel right. The idea is to protect ourselves from exposure — so in that case, the gear should resemble the material used for ambulance sheets. What we have is vastly different, and I might as well wear one of my own clothes and report for duty,” Nurse W says. The nurse is among the many healthcare professionals at the facility who’s not had the chance to partake in any of the COVID-19 training sessions provided so far. “Only the ones who were on ‘leave reserve’ till before 9 April could avail them.” A junior resident at RG Kar Medical College and Hospital mentions feeling “hot air pass through the PPEs” provided at their facility. Choosing to remain anonymous, Doctor B — as the individual shall be referred to henceforth — has been posted at the hospital’s fever clinic, where proper PPE arrived only about two weeks ago. “We are all in this together, but if doctors don’t have the required armamentarium to deal with this crisis, who will it benefit? The OPDs are running normally everywhere across the board, without PPE in most of them. For example, even at the fever clinics at our hospital right now, almost everyone entering is a suspect,” Doctor B says. Even though only a handful of nurses, lift operators, and other ancillary staff are posted at these fever clinics in RG Kar Hospital, they are all operating without protective gear. [caption id="" align=“alignnone” width=“825”]  A photo of RG Kar Medical College and Hospital, Kolkata, taken before the lockdown. Via Facebook.[/caption] Doctor B mentions it’ll be interesting to see how many healthcare workers across the country are taken sick with the virus, in spite of following government orders on PPE, after over seven personnel from RG Kar Hospital were admitted to MR Bangur on testing positive. “The PPE we have aren’t the triple-layered foolproof ones,” the physician says. Arun Agarwal of Green Packaging House, a Kolkata-based manufacturer and supplier of PPE weighs in, mentioning how their gears are made of non-woven material, disposable after a single use. “These are made specifically for the coronavirus, and are waterproof in nature, but cannot be reused,” he says. But security guards posted at the North Bengal Medical College and Hospital (NBMCH) in Bengal’s Siliguri — a testing centre — have been advised to do otherwise. Armed with two sets of PPE each, the guards — stationed at the first entry point for all categories of patients into the facility — have been asked to alternately use each set, washing them on returning home. “Right now, at least the doctors, nurses and other staff coming in direct contact with COVID-19 suspects or positive patients are being given proper PPEs,” says a doctor — who wished to stay anonymous, and will be referred to as Doctor C hereon — posted at a COVID-19 Intensive Care Unit in NBMCH. Earlier last month, the institute made national headlines after reports emerged of doctors and medical staff at the facility being provided raincoats instead of PPE. Subsequently, in a bid to tackle this statewide surge in demand for Personal Protective Equipment, the Mamata Banerjee government roped in Tantuja, — a leading saree and textile manufacturer under the West Bengal State Handloom Weavers Cooperative — who reconfigured their existing machinery to meet prevailing needs. According to Doctor C, the situation at NBMCH has improved, albeit marginally, with PPE kits being carefully rationed by hospital management at present. “Initially, we were also being given PPE that’s used while treating HIV patients, which do not prevent droplet transmission since they only block out blood,” he says. Doctor C hails from Kolkata and has ageing parents who haven’t seen him in months. The presence of a diabetic father at home — who’s especially vulnerable to infections — makes the medic doubly unsure about returning to his family any time soon, even after the lockdown ceases. The fact that he works in a ‘high-risk zone’ only adds to his family’s piling anxiety. [caption id=“attachment_8302361” align=“alignnone” width=“825”]  Rainwear given to healthcare professionals in Kolkata to be used as PPE while dealing with COVID-19 patients.[/caption] [caption id=“attachment_8302371” align=“alignnone” width=“825”] 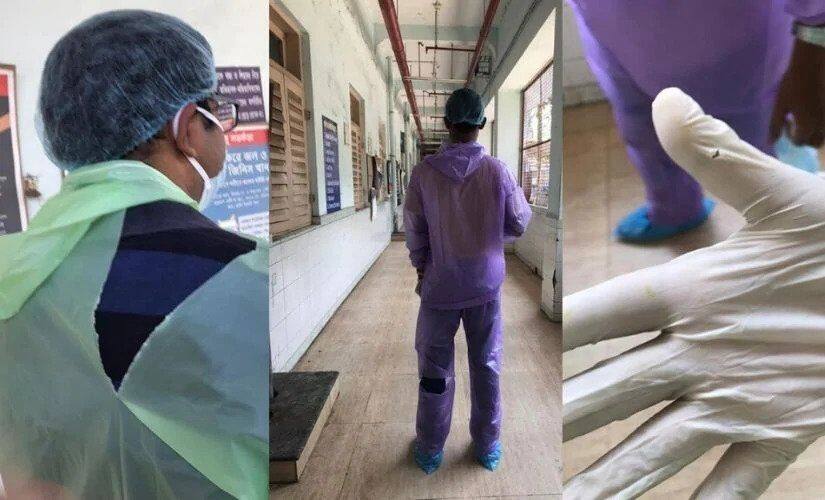 Even the rainwear that was provided with to be used as PPEs was of poor quality.[/caption] **Click here for Coronavirus Outbreak LIVE Updates** “A couple of doctors from the anaesthesia department have been tested and have emerged negative. However, these tests aren’t being done routinely as of now. One doctor, three nurses, and one technician from our hospital have tested positive so far, so it’s really anybody’s guess as to what will happen tomorrow. Right now, we are all grappling in the dark and are novices. Primary symptoms (of the disease) have also changed over the weeks,” Doctor C says, adding that even though he has been taking hydroxychloroquine as a preventive drug, — after the ICMR suggested it might be effective against the coronavirus — he “still can’t be completely sure” of being immune to the contagion. He is currently residing at his college hostel, where cleaners have been debarred from entering, but kitchens and bathrooms continue to be shared by boarders. Medical personnel at NBMCH, barring the ones working in the general medicine wards, have not been granted alternate weeks of ‘quarantine leave’, owing to a lack of proper isolation facilities for the staff. The conversation soon brings us to the long-drawn process of informing concerned parties about a positive test result, where “the test samples are sent to Kolkata from NBMCH in Siliguri for reconfirmation. If tested positive, the patient or even the doctors are not notified immediately, in order to prevent panic, as per a government advisory.” This cautious approach, however, might not be the best way to navigate the prevailing situation in the state, where numbers are reflecting a rapid upswing in the spread. Not only does it prevent authorities from quickly identifying and cordoning off suspects through contact-tracing of COVID-positive individuals, but it also puts healthcare workers at a heightened risk of exposure to contamination. Doctor B from RG Kar Hospital agrees. “We have to be granted more autonomy. If doctors at every level are not given the authority to declare coronavirus-related deaths, and a panel of senior doctors is set up just to vet these things and look at the comorbidities, — besides not being allowed to even communicate who’s a positive case and who’s not — our job only becomes more difficult.” That apart, precious time is being lost too. Currently, West Bengal features among the largest states in the country to have the lowest number of tests being conducted. [caption id="" align=“alignnone” width=“825”]  The entrance to North Bengal Medical College and Hospital, Siliguri. Via Wikimedia Commons.[/caption] According to the COVID-19 data released by the West Bengal government on 25 April, only 9,880 tests have been conducted for the state, which has a population density of approximately 6,915 persons per square kilometre (and a total population of over 90 million). At present, the figures show 423 active cases, 18 deaths, and 105 recoveries in the state.
***
The hours seem to melt into each other, much like one’s skin does underneath the heavy layers of protective-wear, choking the workers by leaving them with no room for eating, drinking water, or even urinating. Right now, the world outside seems identically dreary and suffocating for these individuals, leaving much to be desired at their workplaces. At MR Bangur Hospital, Nurse W alerts me to the congestion occurring at a male isolation ward, where the stipulated distance of one metre is not being maintained between consecutive beds. “This obviously increases chances of infection, rendering the practice of wearing PPE futile,” the nurse says. With roughly 104 beds divided into two halves in the said ward, crowding in this heat only adds to the discomfort of both hospital staff and patients, making the latter restless and unruly at times. “It becomes difficult to control them, especially the male patients,” Nurse W says. Moreover, hospital stairways have been blocked off, leaving people with no option but to use the elevators for commuting up and down the building. Nurse W admits that this measure is counterproductive. With both protected and unprotected individuals availing the same elevators, increased chances of contamination within cramped spaces only exacerbate the situation. “I really hope the staircases are made available again.” One of Nurse W’s colleagues at another COVID-19 isolation ward in MR Bangur Hospital, who chose to remain anonymous as well — and shall be referred to as Nurse X — was recently sent into home-quarantine for 14 days. Nurse X came in direct contact with a colleague who tested positive for the virus on 17 April, but the former subsequently tested negative. “And thank god for it,” Nurse X heaves a huge sigh of relief. The healthcare worker lives alone in the city, with family residing in a neighbouring district. The nurse informs me about the informal system adopted by the nursing staff at the facility, where each one takes turns to attend to patients in PPE, before or after which they do administrative work without the gear. “This ensures that no one has to spend more than three or four hours in the PPE, as it becomes impossible to be in one for more than that,” Nurse X says. The professional was among the many who missed the COVID-19 training sessions, thereby learning everything on the job. “It was difficult initially, as I do not work at the general medicine ward. But now I have gotten used to it,” the nurse says. In these hours of crisis, as healthcare systems race against time to save lives, a resident doctor at the School of Tropical Medicine (Kolkata), — currently posted at Beliaghata ID and BG Hospital — stresses on the importance of sharing knowledge freely within the medical community. “Since there’s barely any time to give proper training to everyone amid this crisis, it’s crucial that we ensure that donning and doffing of the PPE is done in the presence of someone who knows the method, at least for the first couple of times,” the doctor, speaking on condition of anonymity — and who’ll be referred to as Doctor D henceforth — mentions. He points to the fact that just providing protective-wear, without educating healthcare workers on proper disposal methods, makes the exercise futile, as chances of contamination owing to incorrect doffing are rather high. [caption id="" align=“alignnone” width=“825”]  An image of the entrance to Beliaghata ID and BG Hospital in Kolkata before the lockdown. Via Wikimedia Commons.[/caption] “Presently, I am quarantined at my home, living in a separate area away from my family. I come from a family of doctors, so it wasn’t difficult to persuade them into letting me go to work, but in spite of that, the first few moments at Beliaghata ID Hospital were quite nerve-wracking,” says Doctor D, who’s trained in dealing with infectious diseases like HIV, and doesn’t see this crisis as “something very unknown”. He too, however, advises in favour of aggressive testing, especially now that the country is said to be teetering on the edge of Stage 3, or community transmission of the virus. “Since we are working with proper PPE (at Beliaghata ID and BG Hospital), we don’t really need to be tested. But every frontline worker — whether doctors, nurses or paramedics — needs to handle all patients with proper PPE. Currently, most young people are asymptomatic carriers, and we have no idea as to who’s carrying the infection,” the doctor says, adding that door-to-door testing at hotspots is the only way to flatten the curve. His professors asked him to keep calm while on duty, advising him to treat COVID-19 patients the same way he would treat individuals with any other infectious disease, but “with PPE on”. That, Doctor D believes, is the only discernible, yet key difference this time around. Fear has long fled his body. “After a point, you just want to go out and do your job and save lives,” he says. However, chest specialist Dr Kaushik Chowdhury, who’s leading the COVID-19 operations at Beliaghata ID Hospital, holds a different opinion about the young healthcare professionals in the field. According to Chowdhury, less than one-fourth of the workforce is motivated to perform their duties, with mounting anxiety plaguing minds. “We constantly have to remind the doctors, nurses and even the group D staff, that they need to have their spirits up. We, the senior doctors who opened the COVID-19 wards at this hospital, have to keep showing the way by boosting their morale every day,” he tells me. Buttressing this panic are several factors, including fear of contamination during sample collection and interaction with at-risk colleagues working in positive wards. “Besides, there’s the social aspect as well, where many people from the medical community are being ostracised or thrown out of their apartments on account of working on the frontlines. Some are afraid to spread the virus to their families,” Chowdhury says. He observes that most doctors from different medical colleges currently posted at his facility are only doing their jobs out of compulsion, “finishing off their quota of six hours and leaving in a hurry”. While some, he says, are reasonable and rise to the occasion on realising that an uptick in the cases might result in their own colleges being converted to COVID-19 centres overnight, others continue to be saddled with trepidation. “The contagion will likely spread everywhere, and even PPE can provide a limited amount of protection. It’s this knowledge that’s making them nervous, but we are trying to motivate them on a regular basis,” he says, adding that the hospital has employed a team of psychiatrists and psychologists to counsel doctors, nurses, and group D staff through the crisis. Dr Sisir Naskar, Superintendent at MR Bangur Hospital, echoes Chowdhury’s thoughts. “The process of keeping people’s spirits up and fighting the social stigma is constant through this pandemic,” he says, refusing to divulge any further information about the cases being handled at his hospital. For a nurse — who wished to stay anonymous, and will henceforth be referred to as Nurse Y — working at the IPGMER and SSKM Hospital, this stigma is a reality disrupting the lives of co-workers. Nurse Y expresses concern over the issue of several group D staff of SSKM Hospital being expelled from their living quarters in the past few weeks, resulting in very few cleaners showing up for work and adding to the collective distress looming over the facility. “What else will they do?” the nurse asks. [caption id=“attachment_8302351” align=“alignnone” width=“825”]  A photo of IPGMER and SSKM Hospital, Kolkata, taken before the lockdown. Via Facebook.[/caption] Nurse Y, a single parent, left home a day before the lockdown in India ensued on 24 March, and has met his/her school-going child (who’s currently living with an acquaintance) only once ever since. Home, right now, is a distant reality for Nurse Y, whose new address is a quiet corner in the hospital. That’s where the nurse has been living for over a month now, and the end date is nowhere in sight. “There’s no option but to live in the present. I don’t know what will happen tomorrow to me or my child.” For his/her colleague, — who too wished to remain anonymous, and will be referred to as Nurse Z — the pressure to keep one’s lips sealed from higher-ups is unimaginable. “We are only allowed to use PPE when a patient is confirmed as a suspect, and samples have to be collected. Until then, our interaction with the individual is absolutely unprotected,” Nurse Z rues. Test reports aren’t conveyed to them either. “I guess the situation is a little better than before, and we aren’t being given raincoats anymore. But still, there’s a long, long way left to go,” the nurse concludes, poignantly underlining the plight of a world in the throes of a deadly novel pandemic that seems far from over.


)

)
)
)
)
)
)
)
)



