Statistics reveal that two percent of children in India miss their vaccinations either due to ignorance or because of some personal beliefs of their family. Such cases are seen largely in the central and northern parts of India. Most of these cases can be put down to illiteracy, lack of awareness about the need for vaccination and often to lack of time to go to the public health centres and get children vaccinated as the parents are poor and cannot miss a day’s daily wages. However, when a stray case of a child missing vaccinations is seen in a city like Mumbai, with no justifiable reason of poverty or ignorance, then it is a cause for alarm, said Dr Nitin K Shah, consultant pediatric haemato-oncologist at the PD Hinduja Hospital and Medical Research Centre, Mumbai. A 10 year-old who came to visit the doctor recently was from an upper middle class family. She was diagnosed with diphtheria. She had taken a dose of vaccines and missed the rest. The father replied defensively that the family had forgotten to take all the mandatory vaccinations. The mother told Shah in private that the father did not have any belief in vaccinations. The World Immunisation Week is being celebrated from 24-30 April 2019 to promote vaccination to protect people of all ages against diseases. The Union Health Ministry launched Mission Indradhanush on 25 December 2014, and during the first three phases, 28.7 lakh immunisation sessions were held, in which more than 2.1 crore children were reached and 55 lakh of them were fully immunised. In addition, 55.9 lakh pregnant women were also vaccinated with tetanus toxoid. [caption id=“attachment_4866911” align=“alignleft” width=“380”]  Representational image. Reuters[/caption] However, there is nothing much doctors, health workers or the government can do when some people hesitate to get themselves or their children vaccinated, said Shah. “The family has two other children and they were not given all the vaccinations either,” he said. According to WHO, there are more than 19 million unvaccinated or under-vaccinated children in the world. This puts them at serious risk of potentially fatal diseases. By 2017, 123 countries had reached at least 90 percent coverage of DTP3 vaccine. An additional 1.5 million deaths could be avoided, however, if global immunisation coverage improves, it said. Shah spoke to Firstpost on the fears and phobias against vaccination and the fallouts of not getting vaccinated. Excerpts from a conversation with Shah Why are vaccinations important? Immunisation is a child’s birthright and it is the duty of the parents to ensure children are vaccinated. It is also the duty of the healthcare authorities like doctors, nurses, healthcare givers, besides the government, to ensure children are vaccinated so that they are protected from diseases and disabilities. Vaccination provides protection against diseases like diphtheria, hepatitis B, measles, mumps, pneumonia, polio, rotavirus diarrhoea, rubella and tetanus among others. I don’t understand why some people are averse to vaccination. It isn’t that the vaccines are expensive. They are given free by the government in the public health centres. Soon after this government came to power, it launched Mission Indradhanush and recently launched the ‘Intensified Mission Indradhanush’ or IMI so as to reach every child below the age of two years and pregnant women who are still uncovered under the routine immunisation programme. The government data says 82 percent was covered by Mission Indradhanush which means 18 percent did not take vaccination for some reasons. That is a huge percentage who are now vulnerable to illnesses that could have been easily prevented. [caption id=“attachment_6525041” align=“alignnone” width=“825”] 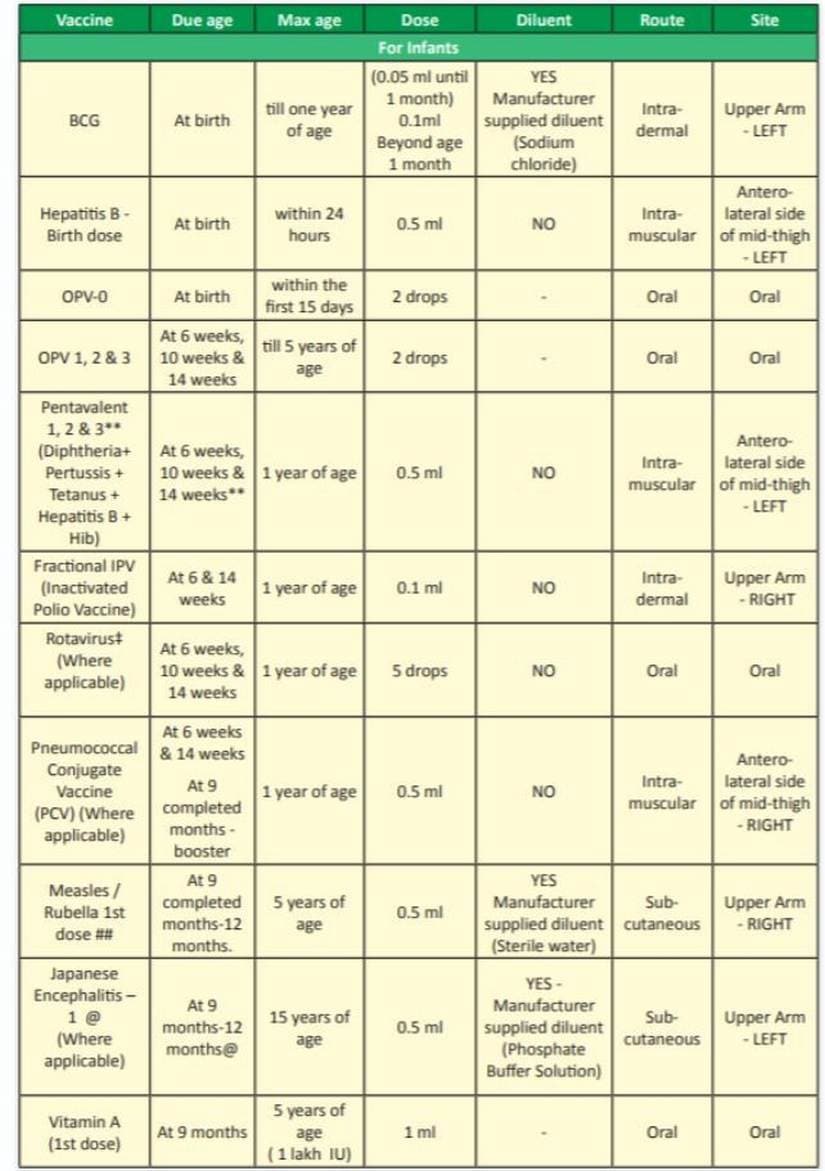 Immunisation schedule for children. Ministry of Health and Public Welfare.[/caption] But the apathy to vaccination is nothing new, is it? The apathy towards vaccination is there even in the United States, for instance. The apathy towards vaccination in the US and India are for different reasons. In the west, vaccine hesitancy is fanned by anti-vaccine lobbies that misguide people through articles, blogs, etc. Cases of measles have increased in the US, for instance, due to hesitancy to take vaccines. In India, people generally follow public health messages and do what is being told to them. Vaccinations are not taken or missed in India primarily because public health centres are too far, and due to personal beliefs or religious reasons for not taking them. How do you think this apathy can be overcome? We can tackle this issue through public health messages, through doctors – when we have children come to us with illnesses, we can talk to their parents about vaccinations and educate them about it. Doctors can have vaccination leaflets, posters in their clinics, in hospitals so that the message is conveyed. Another way of getting around this critical issue is to have a vaccination chart that has a contact of health workers in the area. Mass media can be used as it is being done now so that more people are aware and take vaccinations. When people don’t take vaccinations for religious reasons, we can speak to ask doctors of the same religion and also talk to religious heads. Together they can speak to people of the religion, if it is religious faith that is making them hesitant to take vaccinations. Outreach programs can be conducted. A child cannot speak for herself. But a child saved is an adult saved for the future. From around five to six vaccines earlier to 13 now, we have come a long way. From early 60s to early 2000, there were only 6 antigens for tuberculosis, TPT (against Typhoid, Paratyphoids A and B and Tetanus), measles, etc. We have now added hepatitis B, HIB (Haemophilus influenzae type B vaccine), DPT (diphtheria, pertussis (whooping cough), and tetanus), injectable polio vaccinate, MR vaccine after the campaign; and in some areas we have the rota vaccine against severe diarrhea in children. Beside, PCV (pneumococcal conjugate vaccine) has also been added to the national program. Some areas in the country are highly endemic to Japan encephalitis virus, and Japan encephalitis vaccine is given in these areas. We have replaced the old rabies vaccine with modern tissue culture. The 13 vaccinations a child needs to have are: diphtheria, pertussis, tetanus, polio, measles, hepatitis B, Japanese encephalitis, encephalitis, tuberculosis, pneumococcal disease, haemophilus influenza type B related illnesses, diarrhoea caused by rotavirus, and rubella. The vaccines are offered free by the government. In private clinics, the PCV vaccine costs Rs 2,000 to 2,400 and the rota vaccine is available between Rs 800-1,500. Typically vaccines come to the private market and take a decade or more before it can be provided for public health. The rota vaccines for instance was available for public health in Africa less than a year after it was available in private practice. However, it took us over a decade to get it here.
The World Immunisation Week is being celebrated from 24-30 April 2019 to promote vaccination to protect people of all ages against diseases.
Advertisement
End of Article


)

)
)
)
)
)
)
)
)



