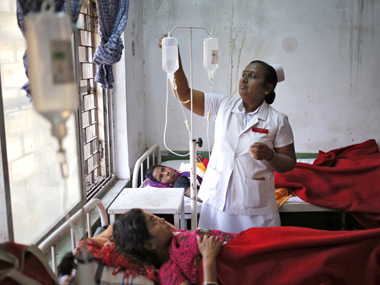
Editor’s note: The deteriorating state of public healthcare in India means that an increasingly larger percentage of its citizens are being driven to the private sector for their medical needs. Mounting costs and decreasing availability of drugs is a major issue, but that’s only the surface of the crisis that confronts the country. The following is the third in a three-part series that looks at a handful of factors that have hampered access to private healthcare in India. The Rules of the Clinical Establishment Act, 2012 required the central government to set a range of rates for medical procedures and services. But five years after the law was passed, neither the central nor any state government has done so. Though the Act is by and large about setting standards for clinical establishments, it does mandate accountability of private healthcare providers by asking them to display prices prominently. The contentious issue of defining the price of healthcare services and procedures has been taken up in many meetings of the National Council for Clinical Establishments, a body that overlooks the entire implementation of the Clinical Establishment Act. But no action has been taken so far. [caption id=“attachment_4333695” align=“alignleft” width=“380”] Representational image. Reuters[/caption] Officials of the Indian Medical Association or IMA, have since then raised objections to the implementation of the Act, including the defining the range of prices. The Act has been adopted only in a total 16 states and Union Territories. But despite them adopting it, most aren’t implementing the Act. “Except some states such as Assam and Puducherry, most states are not implementing the Act,” said Dr Anil Kumar, deputy director-general, the directorate of health services, India. In December 2014, the Ministry of Health and Family Welfare held a sub-committee
meeting for defining the range of rates of procedures and services under the Clinical Establishment Act. In this meeting, it was decided to further make groups in order to carry on the exercise to fix the range of rates for medical procedures and services. But the entire activity soon fizzled out. “We have provided the state governments with a standard
template of costing of procedures including the methodology,” said Kumar. “We are conducting a costing exercise at the central level, but IMA opposed it.” IMA is legally represented in the National Council for Clinical Establishment Act. In the 2014 sub-committee meeting, Dr Vijay Aggarwal from the IMA said that prescribing a range of rates “is against the constitutional right of freedom to practice and hence it is ultra vires and also takes away the independence of the profession.” Representatives from the corporate hospitals said that the management of corporate hospitals decided the rates based on input costs, market forces and price wars. Since there was no control on input costs like costs on establishment, material, costs of living in different areas etc, there is “no use fixing the output/outcome costs,” they opined.
The fact that the costs are based on market forces is precisely the problem. The healthcare market is skewed. The NPPA termed the problem “information asymmetry” between the patient and doctor/hospital, which results in patients being pushed to financial misery.
“Most of the hospitals do not seem to have done a logical costing exercise,” said Malti Jaswal, chief operating officer, Health Insurance TPA of India Ltd. “So far, they have only looked at market-based pricing.” The fact is that the private health industry has never participated in a costing exercise. “None of us has participated in a costing exercise,” said Dr Giridhar Gyani, director-general of the Association of Healthcare Providers, India. “We need to do an activity based costing accounting even for nursing, security, among other factors.” And because hospitals do not know what each procedure costs, they find it convenient to have big markups on pharmacy bills, believes Gyani. “Since we do not know the cost of each procedure, it is easy to cover up the approximate costs by buying medicines in bulk and charging MRP. These margins sustain the hospital.” Some attempts at independent costing studies have been made in the country over the past years, without much success in clearing the perceptions (that private healthcare costs are too high) as its an extremely complex exercise, said Shobha Mishra Ghosh, assistant secretary general of Federation of Indian Chambers of Commerce and Industry (FICCI). The studies, Ghosh said, showed that the rates paid by central government health scheme and various other state health insurance schemes fall short of the actual cost incurred by the private providers. “FICCI is now planning a detailed costing exercise for hospitals across the country to determine average costing modalities and cost inputs under various components to help streamline reimbursements as well as pricing of healthcare services,” Ghosh said. Some patients’ relatives have spoken out against the arbitrary pricing of private hospitals in the recent past. This year, Jayant Singh, whose seven-year-old daughter Adya died of dengue shock last year, filed a writ petition in the Supreme Court seeking the setting up of guidelines to regulate or monitor targets set by corporate hospitals, differential pricing of drugs, and the functioning of pharmaceutical companies and diagnostic laboratories. The petition has been admitted and will come up for hearing in May.
After years of advocacy, the government is now thinking about capping trade margins of medicines and consumables. In April, the government’s think-tank, Niti Aayog recommended the capping of trade margin of a total markup through the trade channel of 24 percent to all traders including stockers, wholesalers stockists, wholesalers, distributors or hospitals for scheduled, essential drugs. The markup would be restricted to 30 percent for non-scheduled drugs.
Activists welcomed the proposed trade margin capping. “However, it is not sufficient to address the problem of high prices because the retail prices will not necessarily be impacted,” said Malini Aisola, from All India Drug Action Network. This means that while the trade margin can be capped, the maximum retail price can still be fixed at a higher price by the manufacturer. She added that the government needs to fix a ceiling price on all life-saving medicines, beyond the 871 essential, scheduled drugs, medical devices deemed as drugs and commonly used consumables. For instance, meropenem, a broad spectrum antibiotic is one of the last lines of antibiotics given to a patient. However, in the case of Adya Singh, the hospital charged Rs 499 at one time for meropenem, and Rs 3,112 another time. They were two different brands. Dr Arun Gadre, from the non-profit Saathi, a health rights advocacy group based in Pune, was part of the sub-committee that worked on the setting of the price range for medical services and procedures and had come up with a calculator. Gadre ran a small nursing home and had first-hand knowledge of how prices can be fixed. The calculator, that he prepared, made certain assumptions that doctors will earn a fixed respectable salary and the price margins should not be more than 20 percent, without making the business unprofitable. The committee did not sit again to work out the details. Gadre feels that the current approach of the government to just fix prices of scheduled drugs and devices will not help. “That is a piecemeal approach,” said Dr Gadre. “Out of five variables, if you control just one variable, the price of healthcare will not come down. Once we agree upon a costing mechanism, then there will be some room for negotiation with the private providers.” Jaswal agrees. She said, “There is a need for the healthcare industry to look at its costing structure and appreciate that India is a mass market wherein everyone would benefit by reasonably priced services rather than higher priced services affordable for few. The upward spiral – of care level and cost, both need to be contained for long-term sustainability.” Read Part I in the series about artificially inflated cost of medicines Read Part II of the series about how industry is bypassing government's efforts to make healthcare affordable


)

)
)
)
)
)
)
)
)



