The contamination of oral polio vaccine reported last week has increased concerns among doctors because of the constant shortage of a safer injectable polio vaccine in the country for the past two years. The injectable polio vaccine would have given children protection from any such contamination, say doctors. The Health Ministry
found that a batch of oral polio vaccines was “contaminated” with a strain of virus — type 2 — that has been withdrawn from vaccines globally. The worry is that this batch leaking into the supply of vaccines could be dangerous for children in a community who had never been exposed to this strain before, and didn’t have immunity. India was declared free of wild polio virus in 2014. Oral polio vaccine contains a live, weakened version of the polio virus. The virus in the vaccine replicates in the intestine of a child and is then excreted for six to eight weeks. On the other hand, the inactivated polio vaccine, that is injected, does not have live virus. Both vaccines prompt the immune system of a person to respond as if it were infected by the virus. The Ministry of Health and Family Welfare in their
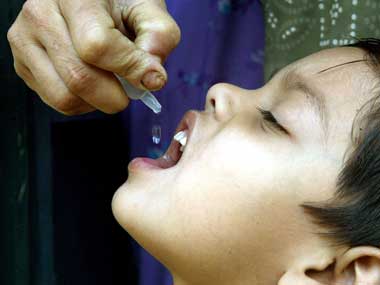
statement said, “As a part of efforts to maintain high immunity against all polio viruses, India provides inactivated polio virus vaccine (IPV) and bOPV to all infants across the country under routine immunization.” [caption id=“attachment_2981532” align=“alignleft” width=“380”] Representational image. Reuters[/caption] However, there has been a major
shortage of the IPV. “A majority of children have not received 2 doses of IPV to protect them from type 2 infection, transmission,” said T Jacob John, a retired professor from Christian Medical College, who has conducted extensive research on polio. “Type 2 (polio virus) is not a risk for the vaccinated child.” Recently, two children from a district in Uttar Pradesh were
admitted to a hospital with acute flaccid paralysis or AFP, a sudden onset of paralysis or weakness in the limbs. One of the causes of AFP could be poliomyelitis, or polio. Traces of type 2 polio virus were found in the samples of their stools, a senior official
told Hindu Business Line. After investigation, the government officials examined the OPV samples which were found to have the type 2 virus. These were traced to Biomed, a Ghaziabad-based pharmaceutical company. Up to 1.5 lakh vials were manufactured by the company, of which two-thirds were administered to children. One-third of the batch has been withdrawn. The batches of contaminated OPV had traveled to UP and Maharashtra,
said government officials. In fact, in August, type 2 polio virus was
found in sewage samples in Mumbai. The government planned a “mop-up” of administering inactivated polio vaccine in specific areas to children who may have missed these doses. Why was polio type 2 strain withdrawn? Before April 2016, the oral polio vaccine had three strains of polio virus — type 1, type 2, type 3 — to prevent acute flaccid paralysis caused by polio. In April 2016, the World Health Organisation called for a
withdrawal of the type two polio virus in the oral polio vaccine globally. The WHO said it was to “eliminate the rare risk of vaccine-associated paralytic polio (VAPP) and circulating vaccine-derived polio virus (cVDPV).” The vaccine-derived polio virus circulates in a community when the virus is excreted from a vaccinated child for more than six weeks. If allowed to remain in the environment, it can genetically change into a form that can paralyse. Vaccine-acquired polio virus occurs when the oral polio vaccine virus mutates in a vaccinated child’s intestine, causing acute flaccid paralysis. This form of polio does not spread. Both these forms of polio cause paralysis. The type 2 polio virus in the oral polio vaccine is most likely to cause the spread and infection of vaccine-derived polio virus in a community, said Dr John. In India, the last such vaccine-derived polio type 2 case was reported in February 2016 in a five-and-half-year-old boy in Bihar’s Siwan district. While withdrawing the type 2 polio virus from the OPV, the WHO introduced the idea of starting the dosage of inactivated polio vaccine in the country. The idea of introducing IPV — which covers all three strains of polio — is to also protect all the children from type 2 polio (which was withdrawn from oral polio vaccine). The inactivated polio vaccine does not cause any sort of vaccine acquired or vaccine derived polio and is therefore safer. Since then, the global health community has been facing severe shortages of inactivated polio vaccine, despite
reassurances from manufacturers over the past two years. It is only this year that the gap of stocks has been filled
to some extent, but many children across India have
missed out on inactivated polio vaccine doses. In India, pediatricians say that IPV is consistently available only in the private sector and is sold as a combination of five of six vaccines, said Dr Vipin Vashishtha, who used to advise the government on the vaccination programme. Concerns of possible vaccine derived polio outbreak Doctors are concerned about the possibility of vaccine-derived polio in the community. “We are at God’s mercy. So far, we have been protected by a large outbreak of vaccine derived polio virus,” said Dr Vashishtha. Between April 2016 and August 2017, five outbreaks of vaccine-derived polio virus type 2 cases were
reported in Nigeria, Pakistan, Democratic Republic of Congo and Syria. The virus can spread via migration, Dr Vashishtha explained. The Health Ministry in its
statement said that children who receive the contaminated vaccine will shed it through their faeces for about 4-6 weeks “after which it will die down.” However, the WHO
said that on rare occasions, if the population is under-immunised, the excreted virus can continue to circulate longer, and in turn undergo mutations. These genetically changed vaccine-virus can paralyse children in the community who are exposed to it. In areas of inadequate sanitation, this excreted vaccine-virus can spread in the immediate community, the WHO
said. To counter this, the government has said that India has made remarkable progress under Swachh Bharat Abhiyan programme. But doctors aren’t convinced. “At this point, there are concerns about the outbreak of circulating type 2 vaccine derived polio virus outbreak as 100 percent children are not immunised with vaccine of all three strains in the country,” said Dr Vijay Yewale, a Mumbai-based pediatrician, and former President of Indian Association of Pediatrics. “Vaccine- derived polio virus is as bad as an wild polio virus infection.”
The contamination of oral polio vaccine has increased concerns among doctors because of the constant shortage of a safer injectable polio vaccine.
Advertisement
End of Article


)

)
)
)
)
)
)
)
)



