An estimated 15 million babies are born too early every year, or in other words, preterm (before 37 completed weeks of gestation). That is more than 1 in 10 babies. Approximately 1 million children die each year due to complications of preterm birth. Many survivors face a lifetime of disability, including learning disabilities and visual and hearing problems. And this number is rising year by year. In India, 27 million babies are born each year out of which
3.5 million babies are born prematurely as per the estimates. This is a tip of the iceberg, as it doesn’t include extreme premature babies. Preterm birth complications are the leading cause of death among children under 5 years of age, responsible for approximately 1 million deaths. According to
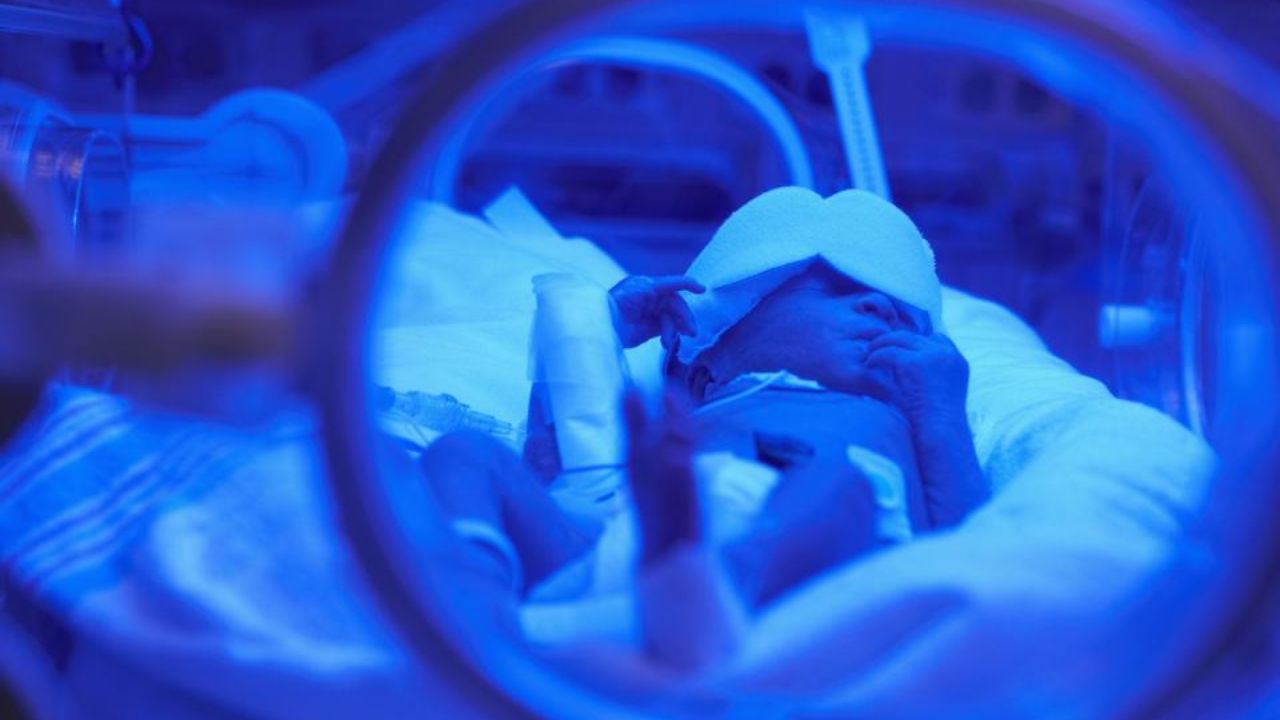
Born Too Soon: The Global Action Report on Preterm Birth, released by Save the Children, The March of Dimes Foundation, the Partnership for Maternal, Newborn & Child Health and The World Health Organization, India tops the list of 10 nations contributing 60 percent of the world’s premature deliveries – with the maximum number of preterm births with 3,519,100 of them, almost 24 percent of the total number. [caption id=“attachment_5546661” align=“alignnone” width=“1280”] A premature baby with jaundice undergoes phototherapy treatment in an incubator. Image courtesy: HNN[/caption] A lack of awareness Preterm birth (PTB) is a significant public health concern and a leading cause of infant mortality and morbidity worldwide and often contributes to various health complications later in life. Several factors such as emotional, stress, social, racial, maternal anxiety, multiple pregnancies, infections during pregnancy, diabetes and high blood pressure, and in-vitro fertilization pregnancy have been shown to be associated with PTB. Data that is emerging also indicated that several occupational, environmental exposure and lifestyle factors might also be associated in part with preterm birth or low birth weight. There is a lack of awareness amongst parents about the understanding of the causes and mechanisms that will advance the development of solutions to prevent preterm birth. The extremely premature babies (born between week 24 to 27) are not even counted by the statistics in India – as the viability is defined in India as 28 weeks and beyond. These babies need advanced neonatal care for them to survive and to survive without disability – we call it intact survival – they need to be delivered in a place with advanced neonatal intensive care units (NICUs) who have the expertise to cater for such babies. This requires a teamwork and expertise not available in all hospitals. [caption id=“attachment_5546681” align=“alignnone” width=“1280”]
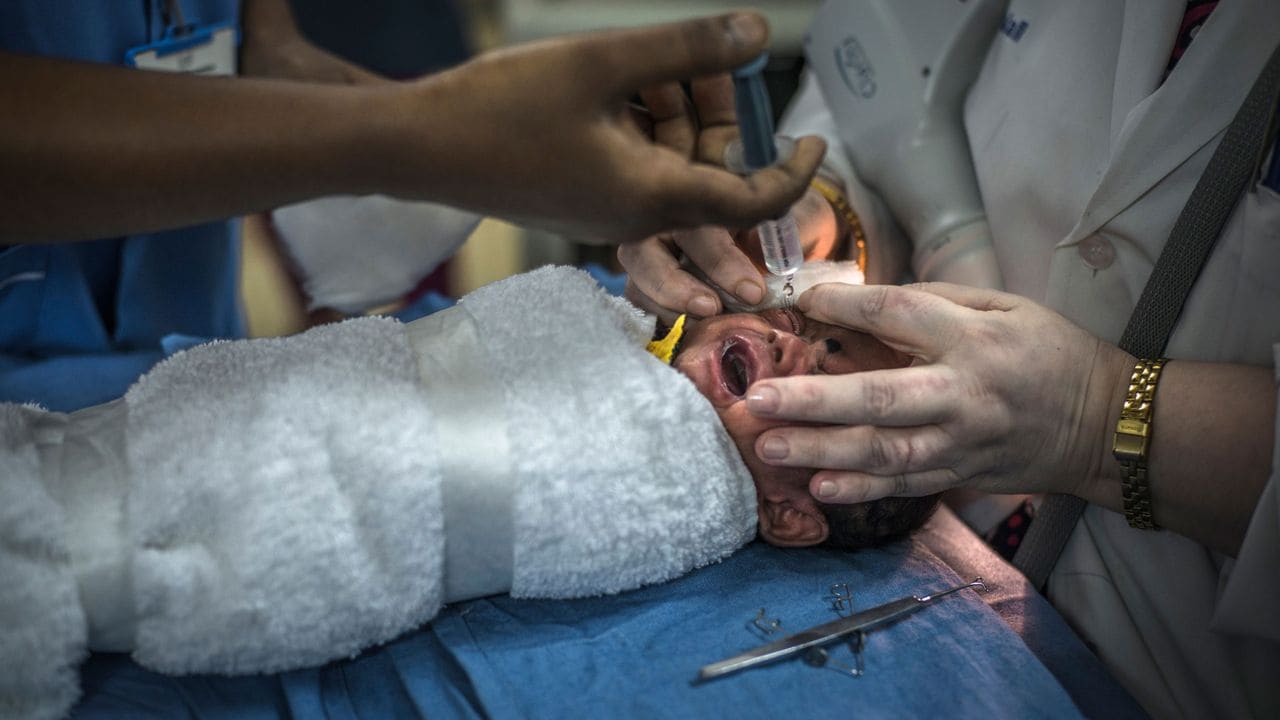 A premature baby with retinopathy of prematurity has dilating eye drops applied a few minutes before he receives laser treatment at Hyderabad hospital. Image courtesy: Time To See[/caption] Generally, as a rule of thumb, both moderate and extremely premature babies should be born in hospitals with advanced NICUs for better outcome – hence most organisations like American Academy of Pediatrics (AAP), Royal College of Paediatrics and Child Health (RCPCH) UK, Indian Academy of Pediatrics (IAP) & National Neonatology Forum (NNF) along with FOGSI (Federation of Obstetricians and Gynaecological Society of India) recommend “in-utero” transfer of babies to the hospitals with advanced NICUs to deliver them there rather than deliver in a place with no NICU and then transfer the baby after being born.This is essential for many reasons including what we call as Golden hour and Golden Day – the first hour of transition from the womb to outside world for these babies is crucial as many babies suffer from brain hemorrhage called IVH (Intra Ventricular Hemorrhage) within the first hour if the babies are not resuscitated properly. The care in the first 24 hours determines their outcome in the next few years of life — whether they survive at all or with or without disability. [caption id=“attachment_5546701” align=“alignnone” width=“1280”]
A premature baby with retinopathy of prematurity has dilating eye drops applied a few minutes before he receives laser treatment at Hyderabad hospital. Image courtesy: Time To See[/caption] Generally, as a rule of thumb, both moderate and extremely premature babies should be born in hospitals with advanced NICUs for better outcome – hence most organisations like American Academy of Pediatrics (AAP), Royal College of Paediatrics and Child Health (RCPCH) UK, Indian Academy of Pediatrics (IAP) & National Neonatology Forum (NNF) along with FOGSI (Federation of Obstetricians and Gynaecological Society of India) recommend “in-utero” transfer of babies to the hospitals with advanced NICUs to deliver them there rather than deliver in a place with no NICU and then transfer the baby after being born.This is essential for many reasons including what we call as Golden hour and Golden Day – the first hour of transition from the womb to outside world for these babies is crucial as many babies suffer from brain hemorrhage called IVH (Intra Ventricular Hemorrhage) within the first hour if the babies are not resuscitated properly. The care in the first 24 hours determines their outcome in the next few years of life — whether they survive at all or with or without disability. [caption id=“attachment_5546701” align=“alignnone” width=“1280”]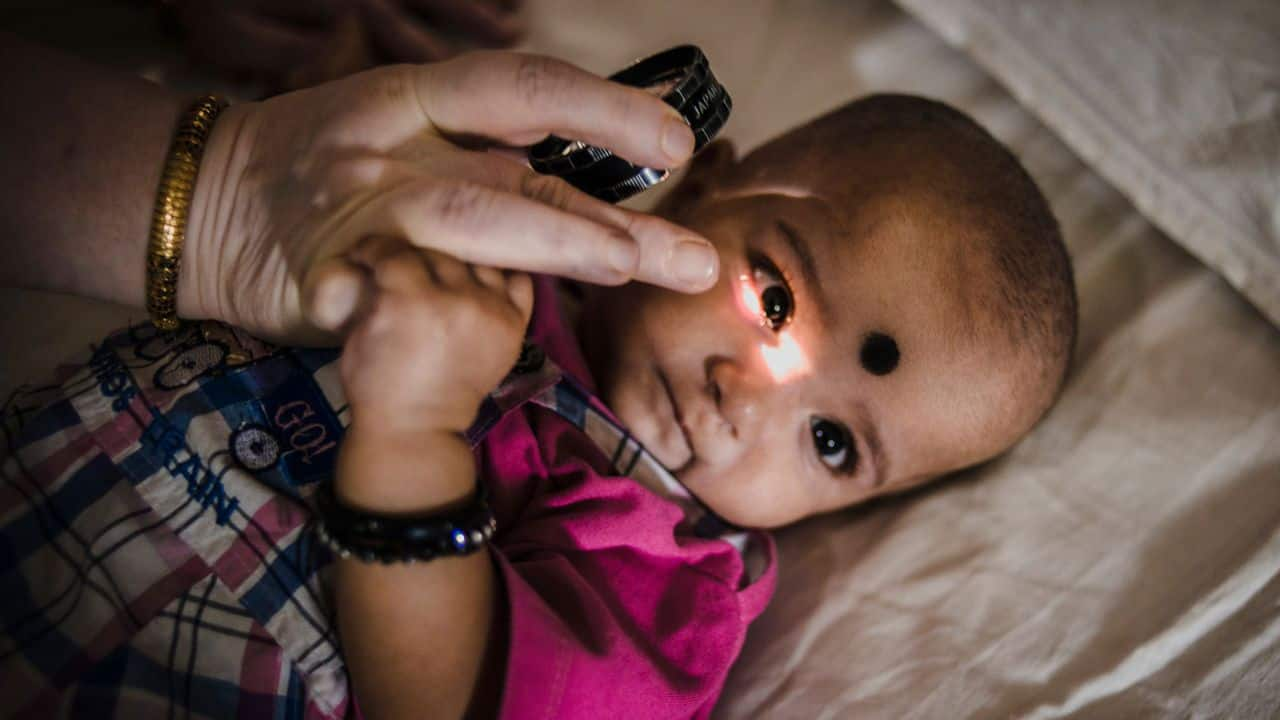 A doctor examines the eyes of a prematurely born child successfully treated for retinopathy in a Hyderabad Eye hospital. Image credit: Time to See[/caption] What does India need to do? Despite several efforts, our systems in India are currently lacking the need for more effort in identifying women at risk of preterm labor and support them to give birth in a health facility that can offer extra care when needed, such as support for adequate feeding with breast milk, continuous skin to skin contact, antibiotics, and antenatal corticosteroids. Inequalities in survival rates around the world are stark. In low-income settings, half of the babies born at or below 32 weeks (2 months early) die due to a lack of feasible, cost-effective care, such as warmth, breastfeeding support, and basic care for infections and breathing difficulties. In high-income countries, almost all of these babies survive. Suboptimal use of technology in middle-income settings is causing an increased burden of disability among preterm babies who survive the neonatal period. Most late preterm babies have higher chances of low temperature (hypothermia) and jaundice requiring treatment (hyperbilirubinaemia) – and if provided proper care, they do well and they may not need to stay in the hospital longer than a term baby in general. [caption id=“attachment_5546771” align=“alignnone” width=“1280”]
A doctor examines the eyes of a prematurely born child successfully treated for retinopathy in a Hyderabad Eye hospital. Image credit: Time to See[/caption] What does India need to do? Despite several efforts, our systems in India are currently lacking the need for more effort in identifying women at risk of preterm labor and support them to give birth in a health facility that can offer extra care when needed, such as support for adequate feeding with breast milk, continuous skin to skin contact, antibiotics, and antenatal corticosteroids. Inequalities in survival rates around the world are stark. In low-income settings, half of the babies born at or below 32 weeks (2 months early) die due to a lack of feasible, cost-effective care, such as warmth, breastfeeding support, and basic care for infections and breathing difficulties. In high-income countries, almost all of these babies survive. Suboptimal use of technology in middle-income settings is causing an increased burden of disability among preterm babies who survive the neonatal period. Most late preterm babies have higher chances of low temperature (hypothermia) and jaundice requiring treatment (hyperbilirubinaemia) – and if provided proper care, they do well and they may not need to stay in the hospital longer than a term baby in general. [caption id=“attachment_5546771” align=“alignnone” width=“1280”] Bilirubin levels are naturally highest 3-5 days after birth. Jaundice, however, is an excess of bilirubin, while affects roughly 80 percent of preterm babies, and more common in breastfed infants. Image courtesy: Mama Natural[/caption] India needs to build upon the infrastructure facilities for improving neonatal survival outcomes at the same time strengthen the tertiary care services at medical colleges, creating secondary care special care neonatal units at district and sub-district health facilities and improving linkages. This is a huge task and needs innovative private-public partnership models, which can facilitate sharing the load taken on by public institutions that have limited capacity to deliver increasing demand for equitable services. In high-income countries, the increases in the number of preterm births are linked to the number of older women having babies, increased use of fertility drugs and resulting multiple pregnancies. In some developed countries, medically unnecessary inductions and Cesarean deliveries before full-term have also increased preterm births. In many low-income countries, the main causes of preterm births include infections, malaria, HIV, and high adolescent pregnancy rates. In rich and poor countries, many preterm births
remain unexplained. Prevention of early birth, however, presents several great challenges. The condition merely describes an event that occurs before its due time and is not a diagnosis in itself. There are many pathways leading to preterm birth and its prevention, each requiring different kinds of scientific inquiry and clinical strategies. Together, they encompass a wide array of measurement systems and clinical interventions across many health-care disciplines that are yet to take hold in Indian healthcare. The author is a neonatologist and Chairman of Cloudnine Group of Hospitals
Bilirubin levels are naturally highest 3-5 days after birth. Jaundice, however, is an excess of bilirubin, while affects roughly 80 percent of preterm babies, and more common in breastfed infants. Image courtesy: Mama Natural[/caption] India needs to build upon the infrastructure facilities for improving neonatal survival outcomes at the same time strengthen the tertiary care services at medical colleges, creating secondary care special care neonatal units at district and sub-district health facilities and improving linkages. This is a huge task and needs innovative private-public partnership models, which can facilitate sharing the load taken on by public institutions that have limited capacity to deliver increasing demand for equitable services. In high-income countries, the increases in the number of preterm births are linked to the number of older women having babies, increased use of fertility drugs and resulting multiple pregnancies. In some developed countries, medically unnecessary inductions and Cesarean deliveries before full-term have also increased preterm births. In many low-income countries, the main causes of preterm births include infections, malaria, HIV, and high adolescent pregnancy rates. In rich and poor countries, many preterm births
remain unexplained. Prevention of early birth, however, presents several great challenges. The condition merely describes an event that occurs before its due time and is not a diagnosis in itself. There are many pathways leading to preterm birth and its prevention, each requiring different kinds of scientific inquiry and clinical strategies. Together, they encompass a wide array of measurement systems and clinical interventions across many health-care disciplines that are yet to take hold in Indian healthcare. The author is a neonatologist and Chairman of Cloudnine Group of Hospitals
India tops the list of 10 nations contributing 60 percent of the world’s premature deliveries: WHO.
Advertisement
End of Article


)
)
)
)
)
)
)
)
)



