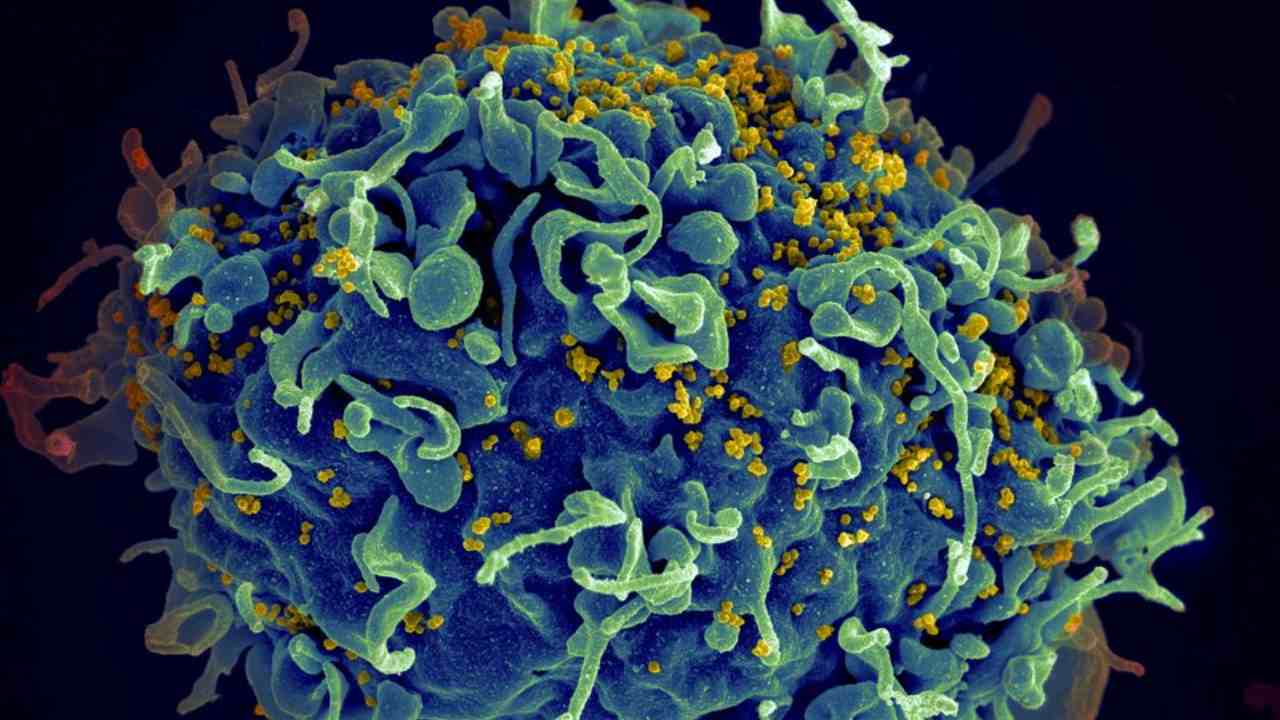
A 36-year-old man in Brazil may be the first to experience long-term remission from HIV after treatment with only a specially designed combination of antiviral drugs, researchers said Tuesday. Just two people have been confirmed cured of HIV so far, both after risky treatments involving bone-marrow transplants for their cancers. The Brazilian patient, who was not identified, has not shown signs of lingering HIV infection in blood tests that detect the virus, according to investigators at the Federal University of Sao Paulo, a prestigious research institution. He also does not seem to have detectable antibodies to the virus. “Although still an isolated case, this might represent the first long-term HIV remission” without a bone-marrow transplant, the scientists said. They presented the results at AIDS 2020, an annual medical conference held virtually this week because of the coronavirus pandemic. But outside experts greeted the report with skepticism. [caption id=“attachment_6200391” align=“alignnone” width=“1280”] HIV virus, in green, attaching to a white blood cell, in orange, as seen under a colored transmission electron microscope. Image credit: NIBSC[/caption] The absence of antibodies to HIV is the most interesting thing about the case, said Dr. Steve Deeks, an HIV researcher at the University of California, San Francisco, who was not involved in the work. “There will be a lot of buzz, a lot of controversy about this part — everyone’s going to be skeptical,” he said. “Am I skeptical? Of course. Am I intrigued? Absolutely.” It is too soon to say whether the Brazilian patient is truly virus-free, Deeks said, until independent labs have confirmed the test results. Even if they do, he added, it is unclear whether the man’s status is the result of the treatment he has received. One in 20 people who start traditional antiretroviral treatment soon after they are infected also suppress the virus to undetectable levels. The patient was diagnosed with HIV in October 2012 and started taking antiretroviral drugs two months later. In 2016, he was one of five people to join a clinical trial in which, in addition to standard drug combination therapy, they received three antiretroviral drugs for 48 weeks. Two of the drugs, maraviroc and nicotinamide, are thought to lure HIV out of its hiding spots in the body, allowing the other drugs to kill the virus. HIV lurks in many so-called reservoirs, and previous studies have suggested that any strategy to rid the body of the virus must include a way to flush it out. Nicotinamide may also boost the immune system, said Dr. Ricardo Diaz, a member of the research team. The patient returned to standard antiretroviral therapy after the trial ended. He stopped taking all antiretroviral drugs in March 2019. His blood has been tested every three weeks since then and has shown no signs of the infection, according to the researchers. “These are exciting findings, but they’re very preliminary,” said Dr. Monica Gandhi, an HIV expert at UCSF and one of the conference organizers. Nicotinamide has been used in many other studies without these results, she noted. And no drug “has worked so far in terms of long-term remission,” she said. “I’m not even sure this has worked. It’s one patient, so I think we can’t say we can achieve remission this way.” The scientists in Brazil have offered to send samples for confirmatory tests to other labs. The researchers should repeat the negative antibody tests, and they plan to do so, Deeks said. The researchers also must test the patient’s blood for antiretroviral drugs, he added: “The data raises the possibility that the participant continued his antiretroviral drugs without informing the study team. This would not be unprecedented.” People in Brazil receive antiretroviral drugs through the public health system, and the transaction is registered, Diaz said at a news briefing Tuesday. “We don’t have a black market, because we don’t need this,” he said. “And there was no registry that this patient got any drugs from the public system.” Still, he said, the team will check the patient’s blood for antiviral drug use that the researchers did not know about. Apoorva Mandavilli. c.2020 The New York Times Company
This could be the first case of long-term HIV remission, without an invasive bone-marrow transplant.
Advertisement
End of Article


)
)
)
)
)
)
)
)
)



