Geneva: Tuberculosis (TB) kills about 5,000 people every day globally with India continuing to take more than a third of the global burden of the disease, new estimates by the World Health Organisation (WHO) reveal. [caption id=“attachment_3051654” align=“alignleft” width=“380”] Representational image. Reuters[/caption] The TB epidemic is larger than previously estimated reflecting new surveillance and survey data from India, according to the
2016 Global Tuberculosis report released on 13 October. India’s TB data are far from flattering by most counts. In 2015, there were an estimated 10.4 million new TB cases worldwide of which six countries accounted for 60 percent of the total burden led by India (25 percent), followed by Indonesia (10 percent), China (10 percent), Nigeria (5 percent), Pakistan (5 percent) and South Africa (4 percent). Of the new TB cases last year, about 56 percent (5.9 million) people were men, 34 percent (3.5 million) people were women and one million were children. People living with HIV accounted for 1.2 million of all new TB cases. In India, 4,80,000 people were killed by the deadly disease (not counting those with HIV and TB). It affected 28,40,000 people (HIV and TB combined) of which 9,95,000 were females and 18,50,000 were males. Although there has been a 22 percent reduction in TB deaths between 2000 and 2015, it killed an estimated 1.8 million people around the world. Of them 0.4 million were co-infected with HIV. A curable disease like TB — which is caused by a bacteria called Mycobacterium — was one of the top ten causes of death worldwide in 2015. It was responsible for more deaths than due to HIV and malaria. India had a case fatality ratio (the proportion of cases of a disease which were fatal) of between 10-19.9 percent. One of the biggest challenges in tackling the disease is the huge gap in testing for TB and reporting new cases. Poor notification is still a problem In 2015, the gap between notifications of new and relapse cases and the best estimate of the number of incident cases was 4.3 million, reflecting a mixture of under-reporting of detected TB cases, especially in countries with large private sectors; and under-diagnosis, especially in countries where there are major geographic or financial barriers to accessing care, the UN’s global TB report says. [caption id=“attachment_3051646” align=“alignright” width=“380”]
India’s TB burden in 2015 as per 2016 Global Tuberculosis (TB). Image courtesy: WHO[/caption] “Some of them (people living with TB) are in fact, never diagnosed, we know that. We are in rural areas, we are perhaps in Mumbai’s poorer areas, yet they go to the private sector or Ayurveda doctors who do not report. So, you don’t even know what the story is,” Dr Mario Raviglione, director of Global TB Programme at WHO said. In India, the non-National Programme for TB (NPT) public sector providers contributed to 16 percent of the total TB notifications while the private sector notified only 11 percent of the TB cases in India. India had the largest gap between new and relapsed notified cases and best estimates of TB incidence in 2015. Multidrug-resistant TB (MDR-TB) remains a public health crisis — WHO estimates that 4,80 000 people fell ill with MDR-TB in 2015. However, again, the geographic distribution of these cases is highly disproportionate with three countries — India, China, and the Russian Federation — carrying the major burden of MDR-TB, which together account for nearly half of all cases globally. “MDR-TB is [what] we keep calling a crisis, which unfortunately, is not being taken seriously enough. Of the new cases, an estimated 3.9 percent have MDR-TB. Roughly, half a million people fell ill with MDR-TB in 2015,” Raviglione added. For the first time, the UN has also done an estimate of MDR and Rifampicin-resistant TB (MDR/RR-TB), defined as resistance to Isoniazid and Rifampicin, the two most powerful anti-TB drugs, for which patients need a second-line regimen. This is significant because it pushes up the total number of people living with drug-resistant TB significantly from previous estimates. Globally, 1,32,120 cases of RR-TB were detected and notified in 2015, and 1,24,990 were enrolled on treatment. [caption id=“attachment_3051650” align=“alignleft” width=“380”]
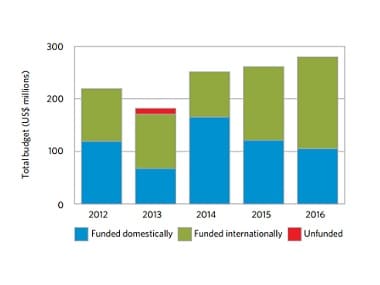 India’s NTP budget as per 2016 Global Tuberculosis (TB). Image courtesy: WHO[/caption] India has a 74 percent success rate of TB treatment, which is much less than the global average of 83 percent, and is behind the BRICS group and other poorer countries of the world. China has a success rate of 94 percent. Even Mozambique (89 percent), Pakistan (93 percent), Tanzania (90 percent) and Vietnam (91 percent) showed better results. Additionally, it has only 46 percent success rate in treating RR-TB. Need more expenditure in healthcare Despite these glaring figures, India relies heavily on international funding for dealing with this public health challenge and its national health budget is much lower than the WHO-recommended levels. In 2014, government expenditures on healthcare were less than the WHO benchmark of at least six percent in 150 countries. India has one of the lowest spending on the healthcare sector globally with a public spending of around one per cent of GDP as compared to three per cent in China and eight per cent in the UK. India’s NTP budget is also one of the lowest among the BRICS group of countries with a spending of about $280 million, only 30 percent of which comes from domestic funding. Compare this with Russia, which has a funding of $1,385 million for countering TB among its population with zero international funding. “It is expected that they (countries with high TB burden) will spend domestically. Four countries out of the five (highest burden BRICS countries) are almost entirely domestically funded. India, that has the largest burden, still requires lot of international support because 60 percent of their funding today is international,” Raviglione said. Two of the indicators reflecting the state of universal health coverage (UHC) are total government spending on healthcare as a proportion of gross domestic product (GDP) and out-of-pocket (OOP) expenditures as a share of total health expenditures. OOP is used as a proxy measure to ascertain the extent to which people lack financial protection to treat TB. OOP as a proportion of total health expenditure as recommended by WHO is at most 15 percent. This proportion is almost 65 percent for India, higher than all BRICS countries and Pakistan. The way ahead WHO lists limited patient coverage, wide variability across states and localities on TB specific-support packages, weaknesses in administration, and no formal links of NGOs as some of the major weaknesses in the Indian counter-TB approach. The world’s available money for spending on TB prevention, diagnosis and treatment in low- and middle-income countries in 2016 was $6.6 billion which is still $2 billion less than the estimates’ requirement for this group of countries in the UN’s Global Plan. At least $2 billion per year is needed for TB research and development but this rate never exceeded 0.7 billion between 2004-2014. The Bacille-Calmette-Guérin (BCG) vaccine, which was developed almost 100 years ago and has been shown to prevent severe forms of TB in children, is widely used. However, there is currently no vaccine that is effective in preventing TB disease in adults, either before or after exposure to TB infection. There are 13 TB vaccines in Phase I, Phase II or Phase III trials. In addition, the rate of reduction in TB cases remained static at 1.5 percent from 2014 to 2015. This needs to accelerate to 4-5 percent by 2020 to reach the first milestone of the World Health Assembly-approved End TB Strategy. Governments have agreed on targets to end the TB epidemic both at the World Health Assembly and at the United Nations General Assembly within the context of the Sustainable Development Goals. They include a 90% reduction in TB deaths and an 80% reduction in TB cases by 2030 compared with 2015. In 2016, four diagnostic tests were reviewed and recommended by WHO. “There must be a massive scale-up of efforts, or countries will continue to run behind this deadly epidemic and these ambitious goals will be missed,” said Dr Margaret Chan, WHO Director General in a press statement.
India’s NTP budget as per 2016 Global Tuberculosis (TB). Image courtesy: WHO[/caption] India has a 74 percent success rate of TB treatment, which is much less than the global average of 83 percent, and is behind the BRICS group and other poorer countries of the world. China has a success rate of 94 percent. Even Mozambique (89 percent), Pakistan (93 percent), Tanzania (90 percent) and Vietnam (91 percent) showed better results. Additionally, it has only 46 percent success rate in treating RR-TB. Need more expenditure in healthcare Despite these glaring figures, India relies heavily on international funding for dealing with this public health challenge and its national health budget is much lower than the WHO-recommended levels. In 2014, government expenditures on healthcare were less than the WHO benchmark of at least six percent in 150 countries. India has one of the lowest spending on the healthcare sector globally with a public spending of around one per cent of GDP as compared to three per cent in China and eight per cent in the UK. India’s NTP budget is also one of the lowest among the BRICS group of countries with a spending of about $280 million, only 30 percent of which comes from domestic funding. Compare this with Russia, which has a funding of $1,385 million for countering TB among its population with zero international funding. “It is expected that they (countries with high TB burden) will spend domestically. Four countries out of the five (highest burden BRICS countries) are almost entirely domestically funded. India, that has the largest burden, still requires lot of international support because 60 percent of their funding today is international,” Raviglione said. Two of the indicators reflecting the state of universal health coverage (UHC) are total government spending on healthcare as a proportion of gross domestic product (GDP) and out-of-pocket (OOP) expenditures as a share of total health expenditures. OOP is used as a proxy measure to ascertain the extent to which people lack financial protection to treat TB. OOP as a proportion of total health expenditure as recommended by WHO is at most 15 percent. This proportion is almost 65 percent for India, higher than all BRICS countries and Pakistan. The way ahead WHO lists limited patient coverage, wide variability across states and localities on TB specific-support packages, weaknesses in administration, and no formal links of NGOs as some of the major weaknesses in the Indian counter-TB approach. The world’s available money for spending on TB prevention, diagnosis and treatment in low- and middle-income countries in 2016 was $6.6 billion which is still $2 billion less than the estimates’ requirement for this group of countries in the UN’s Global Plan. At least $2 billion per year is needed for TB research and development but this rate never exceeded 0.7 billion between 2004-2014. The Bacille-Calmette-Guérin (BCG) vaccine, which was developed almost 100 years ago and has been shown to prevent severe forms of TB in children, is widely used. However, there is currently no vaccine that is effective in preventing TB disease in adults, either before or after exposure to TB infection. There are 13 TB vaccines in Phase I, Phase II or Phase III trials. In addition, the rate of reduction in TB cases remained static at 1.5 percent from 2014 to 2015. This needs to accelerate to 4-5 percent by 2020 to reach the first milestone of the World Health Assembly-approved End TB Strategy. Governments have agreed on targets to end the TB epidemic both at the World Health Assembly and at the United Nations General Assembly within the context of the Sustainable Development Goals. They include a 90% reduction in TB deaths and an 80% reduction in TB cases by 2030 compared with 2015. In 2016, four diagnostic tests were reviewed and recommended by WHO. “There must be a massive scale-up of efforts, or countries will continue to run behind this deadly epidemic and these ambitious goals will be missed,” said Dr Margaret Chan, WHO Director General in a press statement.
Tuberculosis (TB) kills about 5,000 people every day globally with India continuing to take more than a third of the global burden of the disease, new estimates by the World Health Organisation (WHO) reveal
Advertisement
End of Article


)
)
)
)
)
)
)
)
)



