There are now over 537,000 COVID-19 cases worldwide and over 24,000 deaths. The virus that originated in Wuhan in late December has rampaged across the world and penetrated almost every country with cases outside China now far outnumbering those within their borders. [caption id=“attachment_7868241” align=“alignleft” width=“380”]  Representational image. Getty Images[/caption] The recent history of the SARS outbreak in 2002 poses some questions. The genome of COVID-19 is 86% similar to the SARS genome, yet the two strains have played out very differently. It took six months for SARS to exceed 5,000 cases; COVID-19 took a month. SARS resulted in over 8,000 cases in 26 countries and caused 774 deaths (with the vast majority in China and Hong Kong) and then dissipated by July 2003 after extensive containment and isolation measures. Why, then, has COVID-19 proven to be so challenging to contain despite near-global containment measures? Chinese researchers had already shared the sequence of the whole genome by mid-January - this process took longer for SARS - and medical advances in the last 15 years should have prevented this pandemic. Taking a closer look at the differences in the viruses, transmissibility, geographic and historical junctures explains why COVID-19 spread so rapidly and why it has been so difficult to contain.
A bigger city, a more globalized world
Wuhan is a major city with over 11 million inhabitants. It is a major transport and industrial hub. It is home to the largest airport in central China and sees a massive influx of inbound and outbound traffic. China has changed since 2003 as well, it is far more interconnected and population density has increased substantially as well. All these factors make it fertile ground for an infectious disease to spread in great numbers. Some coincidental factors played a role as well - just before the lockdown was announced in Wuhan, more than 5 million people had left the province for the upcoming Spring Festival, spreading the disease all over China. SARS started in the southern province of Guangdong and was contained more to hospital facilities - it simply didn’t spread as much. The area was not as connected and globalized as Wuhan is today.
Transmissibility
Studies have now shown that SARS has a lower R0 value than COVID-19, meaning that an infected person transmits it to fewer people on average. A COVID-19 positive person can transmit the infection to 2 to 3 people on average. The Diamond Princess, the cruise ship with 3,700 passengers, ended up with 700 positive cases while it was quarantined off the coast of Japan. Public health measures had been implemented but could not prevent the outbreak, suggesting that COVID-19 is highly infectious.
The structure of the virus
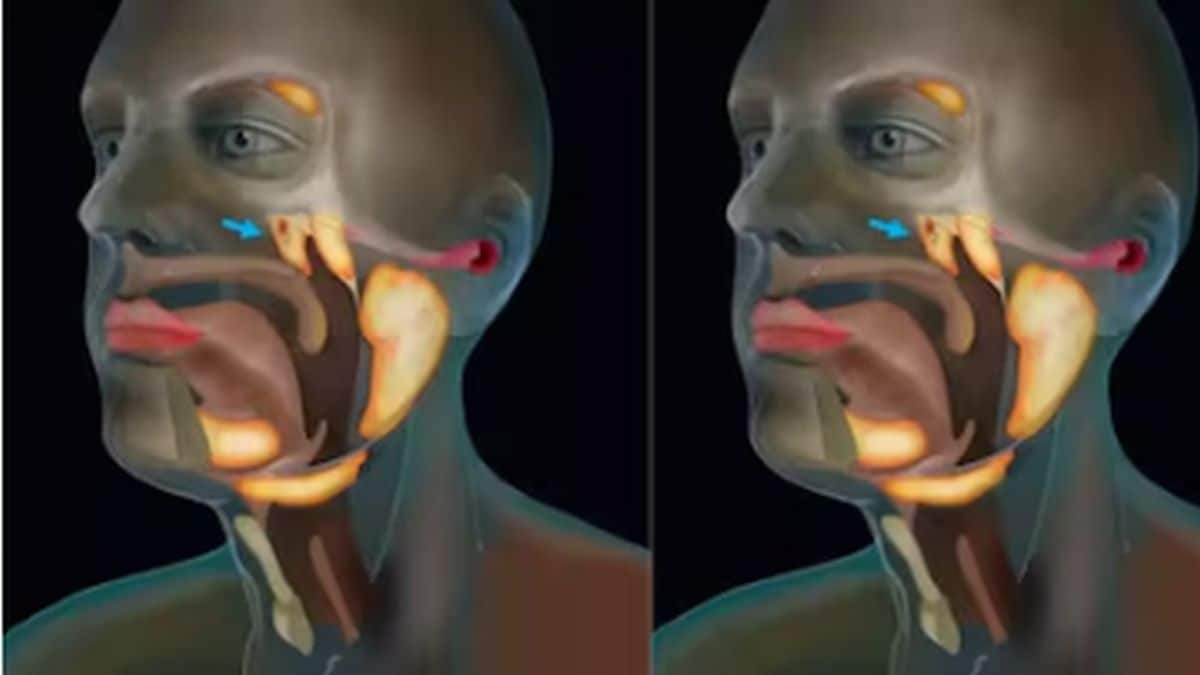
Coronaviruses have a protein called spike on their outer membranes. The spike protein is responsible for identifying living cells and invading them. Spike proteins attach to ACE2 receptors (proteins on the outer layer of cells found in the respiratory tract and other places) to enter a cell and initiate the infection process. It turns out that the structure of SARS-CoV-2 (the coronavirus that causes COVID-19) spike proteins conforms more strongly to ACE2 receptors; the bond is stronger and it is easier for SAR-CoV-2 to invade cells. To dig a little deeper, the spike protein is actually composed of two halves that need to be broken for the virus to invade the cell. SARS-CoV-1 (which caused SARS) had more difficulty engineering this break, whereas SARS-CoV-2 relies on a naturally occurring enzyme in the body called furin to make the cut. Since furin is readily available, the passage of COVID-19 is eased further. These structural differences have a profound impact on the transmissibility of the infection and explain, in part, why COVID-19 is more infectious and likely to spread.
Asymptomatic carriers and mild cases
Perhaps the most significant reason for the spread of COVID-19 is the fact that those with mild symptoms or even no symptoms can spread the disease. This was not the case with SARS with people becoming most infectious only after serious respiratory symptoms appeared. Further, those with mild symptoms were much less frequent in SARS and there were no reports of this subgroup transmitting disease. This underscores why containment and quarantine measures worked so much better with SARS. It was easier to identify those who were sick and infectious and isolate them so they didn’t spread the disease - SARS is also spread through droplets and hand to face contact like COVID-19. In the case of COVID-19, most cases will go unrecorded and it is much more challenging to isolate those with mild symptoms. This is why the WHO urges extensive testing - isolating those who are carriers is the surest way to slow down the pandemic. While COVID-19 is less deadly than SARS in terms of its mortality rate, its strength lies in its sneaky transmissibility… And therein should lie our defence as well. For more tips, read our article on COVID-19_._ Health articles in Firstpost are written by myUpchar.com, India’s first and biggest resource for verified medical information. At myUpchar, researchers and journalists work with doctors to bring you information on all things health.


)
)
)
)
)
)
)
)
)



