Editor’s note: This series will focus on the difficulties faced by the medical fraternity at COVID-19 hospitals, their duty hours, access to protective gear, facilities they get during quarantine, how are their families coping with this new reality across different states in the country. This is the second part of the series.
After working for over a month with spells in quarantine at the Kalamassery Medical College Hospital, Ernakulam which has been turned into a COVID-19 speciality hospital, 32-year-old Ravi Chandran undertook a three hour journey home Palghat district. He was looking forward to seeing his wife and children who had moved to his in-law’s home before the Janata Curfew was announced in March 2020. Chandran works in the administration department of the hospital.
After reaching Palakkad, Chandran was stopped at the gates of the house by neighbours. “A few people gathered and asked me to leave. They argued that since I work in a hospital, I was in danger of carrying the virus. I tried to explain, but could not reason with the crowd that was gradually increasing. I finally decided to leave,” Chandran said. His regret is that he could not hug his children or talk to his wife.
Medical staff risk their lives and expose themselves to the dangers of the COVID-19. Though hailed publicly for their service, they are socially unwelcome once they step out of the hospital premises. The threats posed by coronavirus creates fear and panic and the until-then warm neighbourhood treats medical and other hospital staff as pariahs.
Firstpost spoke to medical and support staff at the Kalamassery Medical College Hospital to understand the stress and the conditions under which they work. They agreed to speak on conditions of anonymity. All names mentioned in this article are changed, as per their request.
Quick Reads
View AllCOVID-19 in Kerala
On 30 January, the country’s first COVID-19 case was reported in Kerala and the State reported its first coronavirus death after a 69-year-old man being treated for the virus died at the Kalamassery Medical College Hospital. The man-from Chullikkal in Ernakulam, was admitted to the isolation ward on 22 March after his return from Dubai. His death was also due to other complications – heart disease and high blood pressure. He had a bypass surgery earlier, doctors at the hospital said.
Click here to read the complete series
As early as mid-January, the Government Medical College Hospital in Ernakulam was geared up for the epidemic. A control room was set up. Kerala has many students studying at Wuhan in China, the epicentre of the coronavirus and there was a fear of them returning and being possible carriers of the virus. It has a well-oiled machinery which has dealt swiftly and effectively against the deadly Nipah virus earlier, which hit the State in 2018.
The hospital has 30 isolation beds and 10 beds have been set aside for suspected cases of COVID-19. It is prepared for 500 beds, in case of an emergency, said Kala Menon, a specialist in infectious diseases.
PPE gear and ‘suffocation’
The hospital has charted a four hour long duty time for staff working in the COVID-19 wards instead of the mandatory 8 hour shifts they worked earlier. The reason for the change in duty hours is not due to the dangers posed by the virus, but due to the heavy personal protection equipment (PPE) gear the staff has to wear.
Once the doctors and staff get dressed in the PPE gear, no one can work beyond four hours. Covering the entire body from head to toe, it restricts movement and is uncomfortable as the body temperature rises once it is worn. While staff have devised their own ways to work with it, the heat generated after wearing the gear is ‘terrible’, they said.
Once the gear is worn, the doctors and staff cannot drink or eat or even visit the washroom. To wear the PPE gear, the staff has to reach the premises at least an hour before the shift begins. There are specially demarcated entry and exit ways for medical staff treating COVID-19 patients.
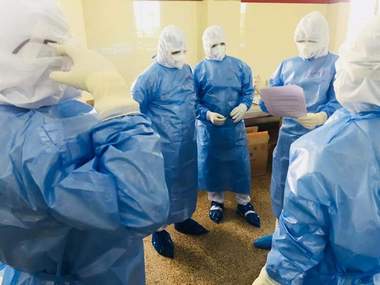
The PPE gear can be worn only with another person’s help. There is an order to be followed while wearing it. Each item of wear is first sprayed with a disinfectant. “We wear the shoes first,” said staff nurse Grace Sebastian. Then the PPE overalls are worn. Most staff wear one or more masks to cover their mouth and nose after which the head is covered. The goggles are worn next and then two pairs of gloves are pulled over the hands. All parts of the PPE gear is securely pinned so that no part of the person’s body is exposed. Since the identity of the person wearing the gear is not known, identification labels are affixed or written on them.
There is also a procedure to be followed for removing the PPE gear. The assistant who helps the staff has to spray disinfectants on the PPE before removing it. Each part of the PPE has to be disposed off in different bins. The cleaning staff does not come in contact with it as they pick up the bins in which the used gear is thrown into and leave it at the waste disposal area.
Life after day’s work
The hospital has set up accommodation within its premises for its staff. After duty, the staff cannot interact with others. Some like senior nurse Ragini Shankaran go home in vehicles arranged by the hospital. “I have two children aged four and six. They have now understood that they cannot come near me once I am home. Earlier, it was difficult for family members to hold them away from me. But it has been over two months now and they stand away at a little distance and talk to me,” said Shankaran, who said she was happy to be able to go home and see her family.
Others are not so lucky. 30-year-old Molly Jose, a staff nurse at the hospital said she felt ‘terrible’ at not being able to meet her children — a two-year-old son and four-year-old daughter — now living with her mother. “I haven’t seen them for over a month now,” she said, her voice shaking.
At first, Jose would talk to her children daily through video calls. But after the few instances when the children started crying on seeing her, she decided to just make voice calls and talk to them. “They don’t cry any more but ask me when I am coming home,” she said.
Haritha Sukumaran, a cardiac surgeon, said that nurses mention these instances when they help doctors to wear the gear. “It is painful for a parent to be away from their children, but no nurse or even support staff is forced to work and can opt out of this duty – everyone understands the gravity of this illness,” she said.
When Molly Jose was asked if she wanted to opt out of the COVID-19 care, she was quick to reply that though she was afraid of catching the virus, just like any other medical staff, she believes that is not a reason to opt out of duty. “We have seen the deadly Nipah cases at this hospital earlier. It causes acute respiratory illness and fatal encephalitis and we were successful in treating it,” she said.
What pains the medical support staff who take care of the patients needs – bringing food, cleaning rooms and disposing off the waste - is the treatment they are meted outside the hospital. For 46-year-old Susheela Venugopalan, who lives with her family a short distance away from the hospital, the memory of the evening she was shooed off at a grocery store evokes pain and sadness. “I had gone after duty-hours to the grocer-who I know for years, and maintained social distance as well. But other customers in the shop asked me to leave. Many of them are known to me,” she said.
When these incidents are brought to the notice of the hospital, the administration lodges a police complaint, as in the case of its staff nurse, Radhika Murali. The 22-year-old decided to live with her sister to make it easier to travel to the hospital with the lockdown in force. When the neighbours saw her in the apartment, they not only asked her to leave but also called the police. Murali called up the hospital for help. The hospital filed a complaint and police were sent to the apartment to speak to the neighbours. However, Murali decided against going to her sister’ house until the virus cases dwindle, she said to Firstpost.
The medical staff work for five days and are then quarantined or live in isolation for 14 days. They spend their time reading or watching films. The cleaning staff is not so lucky though. They follow the same rules of work and quarantine periods, but they are often called back for duty from quarantine if the hospital falls short of staff, said one of the health inspectors at the hospital.
“Not a single person has refused to come to work,” he said. Most of the support staff are temporary workers and earn Rs 600 per day. The health inspector said what makes him proud to work in the hospital is the dedication he sees in everyone tending to the virus cases. “That is commendable,” he said.
One of the health inspectors at the hospital has to be content with seeing his family from far as he cruises off on his bike near his in-laws’ house. “I have shifted my wife and children to my in-law’s house since the Janata Curfew. My younger daughter was born premature and there were some complications after that. The baby is fine now but yet just a year-old. So, most days I go on my bike and call them on the phone when I am near the house. My wife and children then come out and stand in the verandah. I am able to see them for a few minutes and then I return to my house,” he said.
The health inspector shared his angst of returning to an empty home without his family. “On most days the work at the hospital makes it impossible to go home, which is a god-send,” he said. “I miss the children and their laughter at home,” he said.
Joys of working in Kerala
When Veronica finished her MBBS degree and then specialised in the treatment of infectious diseases, she felt most of her batchmates were ‘lucky as they chose to go to the United States of America (USA). “I always felt they lived better lives than me. I had chosen to work in Kerala,” said Veronica.
Veronica’s oft-held belief was decimated completely last week. “My batchmates and I talk regularly on the phone. Last week when I spoke to some of them, they mentioned that they did not have adequate PPE gear. They spoke of their struggling healthcare system. For the first time in my life, I felt very proud of the choice I had made to work here in Kerala.
“The Kalamassery Government Medical College Hospital has more than adequate PPE gear for all of us who treat and care for the COVID-19 patients. We don’t have to worry about these things. We are prepared with a backup of 600 beds if there are more cases. The government has always been very proactive about healthcare in Kerala. There is nothing to be envious about working and living in the US,” she said, laughing.
Another reinforcement came in the form of praise that the hospital and its staff received from a British national who was treated as a virus suspect. Veronica recalls how the Englishman was initially alarmed to stay in the isolated ward.
“On the first day when I went to his room, I found him writing something,” says Veronica. “When I asked him what he was doing, he said he was writing his will. He was afraid of the medical treatment at a government hospital in India, he told me. I tried to comfort him, but he had a terrified expression on his face. A day or two later he started laughing and chatting with medical and support staff who entered his room. When he was discharged, he told me he would not have got such excellent care back home in Britain,” said Veronica.
Indian medical care, particularly Kerala’s has come in for much praise globally. Veronica did indeed make the right choice to be a doctor in Kerala. “Of course, I did,” she said amid much laughter.


)

)
)
)
)
)
)
)
)



