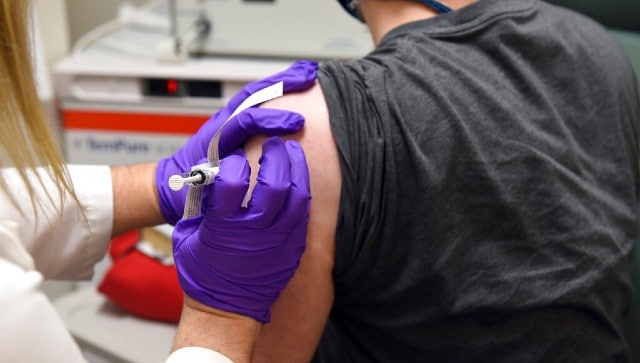
On Monday, AstraZeneca, the third major drug company working on developing a COVID-19 vaccine, reported 70 percent efficacy for its vaccine candidate ChAdOx1 nCoV-19 (AZD1222) developed by Oxford University, while Russia’s vaccine candidate Sputnik V claimed efficacy of over 95 percent 42 days after the first dose. The news has come at a time when most countries across the world are reeling under a fresh wave of the coronavirus pandemic that has pummeled the world economy and led to 14 lakh deaths, 1.34 lakh of which are from India alone. Besides the Oxford-AstraZeneca and the Sputnik V developed by Russia’s Gamaleya Research Institute, two other vaccine candidates have also announced their efficacy rates. The Pfizer-BioNTech’s BNT162b2 has 95 percent efficacy while Moderna-NIH candidate mRNA-1273 is more than 90 percent effective. Efficacy refers to the likelihood that a coronavirus shot will work in people. These efficacy numbers, however, may change as the vaccine studies continue. For example, one regimen of the Oxford-Astrazeneca vaccine candidate demonstrated an efficacy of 90 percent when it was was given as a half dose followed by a full dose one month later. The second regimen showed 62 percent efficacy when given as two full doses a month apart. The average efficacy is therefore 70 percent. Currently, there are 11 vaccine candidates at the last stage of phase III trials, including the four named above. Overall, as per the latest data released by the WHO on COVID-19 vaccines (last updated on 12 November 2020), there are 48 candidate vaccines undergoing clinical evaluation at various stages, whereas, 164 candidate vaccines are in preclinical evaluation. Let’s look at some of the prominent vaccines that are nearing the last phase of trials. [caption id=“attachment_9004121” align=“alignnone” width=“640”] Pfizer vaccines distributed in the US will come from its largest manufacturing plant located in Kalamazoo, Michigan. AFP[/caption]
The Majestic Four: Trojans vs mRNA tech
Pfizer-BioNTech: Earlier this month, Pfizer became the first to announce that its Messenger RNA (mRNA) vaccine candidate BNT162b2 has 90 percent efficacy, drawing applauds from everywhere and criticism from some quarters especially as the logistical challenges that it present in terms of delivery and storage became clear. The vaccine developed by BioNTech completed its phase three trials on 18 November with an efficacy rate of 95 percent beginning 28 days after the first dose. The efficacy, Pfizer said was “consistent across age, gender, race and ethnicity demographics; observed efficacy in adults over 65 years of age was over 94 percent”. During the study, 170 confirmed cases of COVID-19 were evaluated, with 162 observed in the placebo group versus 8 in the vaccine group, it added. Pfizer and BioNTech recently applied to the US FDA for emergency usage authorisation. The companies expect to produce globally up to 50 million doses in 2020 and up to 1.3 billion doses by the end of 2021; the companies will be ready to distribute the vaccine within hours after regulatory approval. In July, the company signed a contract to supply the US with 100 million doses for $1.95 billion under Operation Warp Speed, assuming the vaccine is cleared by the FDA. Based on the two companies’ agreement with the US government, the vaccine is likely to cost about $20. However, more than the cost, it’s the ultra-low temperature storage requirements of the vaccine is likely to play major hurdle in the delivery of the vaccine. One of the downsides of mRNA vaccines is that the mRNA
molecules are fragile, reports USA Today. To keep them from falling apart, the vaccine has to be kept at an ultra-low temperature, ie, below -70 degrees Celsius. At this temperature, the vaccine can be stored for up to six months at ultra-low temperature. Reuters said that the vaccine can also be stored at 2-8 degrees Celsius, the temperature of a regular refrigerator which is most commonly available at hospitals, but this way, the vaccine can last only for five days. [caption id=“attachment_9004111” align=“alignnone” width=“640”] This October 2020 photo provided by Pfizer shows part of a “freezer farm,” a football field-sized facility for storing finished COVID-19 vaccines, under construction in Kalamazoo, Michigan. AP[/caption] This requirement of ultra-low temperature also makes the transport and distribution of the Pfizer-BioNTech vaccine candidate a logistical problem, especially since the vaccine, requires two shots, given several weeks apart. It also remains to be seen how long will the protection last. Neither Pfizer nor BioNTech has signed any agreements with the Government of India or Indian companies to manufacture the vaccine in India. Also, the requirement of the ultra-low freezers makes it unsuitable for a country like India. It’s also unlikely that India may approach Pfizer for the vaccine, as Union health minister Harsh Vardhan recently said that “
India may not need the Pfizer vaccine”. Moderna-NIH vaccine: Developed by the Kaiser Permanente Washington Health Research Institute, Washington, this vaccine is being manufactured by US-based Moderna pharmaceutical. The Moderna vaccine is similar to the Pfizer-BioNTech as both use mRNA technology, however, the Modern candidate doesn’t require ultra-low temperature for storage. Moderna’s vaccine also starts off frozen, but the company said Monday it can be thawed and kept in a regular refrigerator for 30 days, easing that concern. Moderna said its vaccine appears to be 94.5 percent effective, according to preliminary data from an ongoing study. The vaccine too requires two shots given several weeks apart. Moderna’s vaccine is being studied in 30,000 volunteers who received either the real thing or a dummy shot. On 15 November, an independent monitoring board examined 95 infections that were recorded after volunteers’ second shot. Only five of the illnesses were in people given the vaccine.
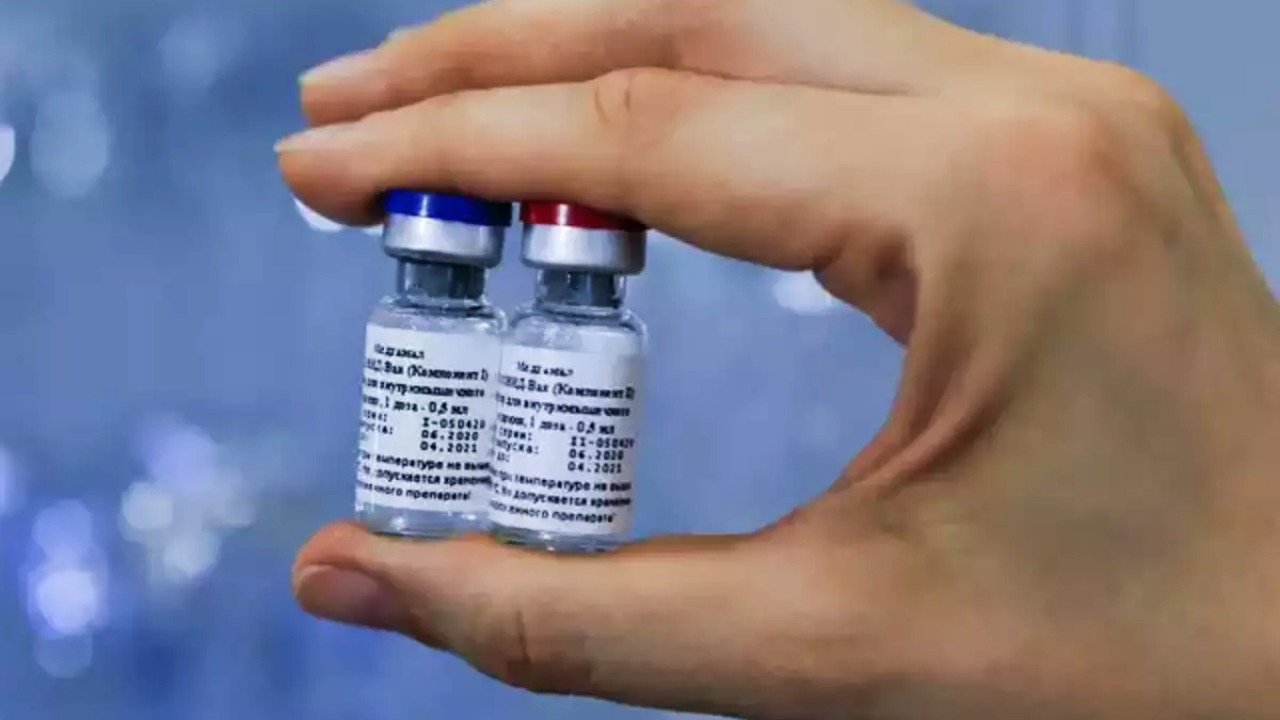
But Moderna’s independent monitors reported some additional, promising tidbits: All 11 severe COVID-19 cases were among placebo recipients, and there were no significant safety concerns. The main side effects were fatigue, muscle aches, and injection-site pain after the second dose. As per reports, based on the companies agreement to sell the vaccine to the US government, the Moderna vaccine may cost anywhere from $15-$25. Though talks are on between the Indian government and Moderna to manufacture the Moderna-NIH vaccine in India, the cost is likely to be a factor. This may be the most expensive vaccine at MRP. Sputnik V: The Sputnik V is an adenovirus-based vaccine developed by the Gamaleya National Research Center for Epidemiology and Microbiology of Russia’s health ministry. In a press release issued on Tuesday, the Russian Direct Investment Fund (RFID), Russia’s sovereign wealth fund, said that the second interim analysis of clinical trial data showed a 91.4 percent efficacy for the Sputnik V vaccine on Day 28 after the first dose, whereas the efficacy is over 95 percent 42 days after the first dose.
EXCLUSIVE VIDEO: #SputnikV vaccine production in Gamaleya Institute, Moscow. pic.twitter.com/VXS5Bd3wKj
— Sputnik V (@sputnikvaccine) November 24, 2020
Russia had approved the usage of the vaccine in August without the completion of trials in Russia, drawing criticism from experts. RFID has said that the lyophilized (dry) form of the vaccine can be stored at +2 to +8 degrees Celsius. The company also announced on Twitter that the cost of one dose of the Sputnik V vaccine will be less than $10 for international markets, and is in talks with manufacturing partners to produce the vaccine for more than 500 million people in 2021.
BREAKING: The cost of one dose of the #SputnikV vaccine will be less than $10 for international markets. RDIF continues expanding existing agreements with international manufacturing partners to produce the vaccine for more than 500 million people in 2021. https://t.co/RHOagQnmA5
— Sputnik V (@sputnikvaccine) November 24, 2020
Currently, trials of the vaccine in 40,000 volunteers are underway in Russia and Belarus. A number of countries, such as UAE, India, Venezuela, Egypt, and Brazil are expected to conduct clinical trials of Sputnik V locally. The RFID has made an agreement with India-based Dr Reddy’s Laboratories to supply 10 crore doses of the Sputnik V vaccine following the successful approval of the Drugs Controller General of India (DCGI). Dr Reddy’s is expected to soon begin adaptive Phase 2/3 trials of the vaccine in India. The
first batch of vials for the trials have reportedly already arrived in India. [caption id=“attachment_8825841” align=“alignnone” width=“640”] Representational image. AP[/caption] Oxford-AstraZeneca: Developed from a cold virus, or adenovirus, that normally infects chimpanzees, by Oxford University the ChAdOx1 nCoV-19 vaccine candidate is manufactured by AstraZeneca. The phase three trials of the Oxford-AstraZeneca candidate showed 70 percent efficacy, which is the lowest of the four major vaccines which have revealed their efficacy data as yet. However, the fact that the ChAdOx1 nCoV-19 vaccine doesn’t have to
be stored at freezer temperatures, makes it potentially easier to distribute, and thus a major breakthrough. The AstraZeneca vaccine can be stored at 2 degrees to 8 degrees Celsius (same as the Sputnik V). The vaccine uses a weakened version of a common cold virus that is combined with genetic material for the characteristic spike protein of the virus that causes COVID-19. After vaccination, the spike protein primes the immune system to attack the virus if it later infects the body. AstraZeneca has told The Associated Press that it will immediately apply for early approval of the vaccine where possible, and it will seek an emergency use listing from the WHO, so it can make the vaccine available in low-income countries. The successful approval of the Oxford-AstraZeneca vaccine is more important for India — both in terms of availability as well as delivery — as a version of the Oxford candidate known as Covishield is being developed by Serum Institute of India (SII) and the Indian Council of Medical Research (ICMR). AstraZeneca, which has pledged it won’t make a profit on the vaccine during the pandemic, has reached agreements with governments and international health organisations that put its cost at about $2.50 a dose, according to The Associated Press. According to a Moneycontrol.com report, SII is expecting to make the
Indian version of the vaccine candidate available for Rs 500-Rs 600 to the public (maximum Rs 1,000 for two doses) in India, reported MoneyControl.com. The Oxford-Astrazeneca vaccine candidate is the cheapest vaccine candidate awaiting regulatory approval.
Other global contenders
NVX-CoV2373: Developed by US-based Novavax, this vaccine will also be manufactured in India as Covovax in association with SII and ICMR. According to an official release, the company has initiated its first Phase 3 study in September in the UK in partnership with the UK Government’s Vaccines Taskforce. The NVX-CoV2373 is a stable, prefusion protein made using Novavax’s recombinant protein nanoparticle technology that includes its proprietary MatrixM adjuvant, the company said in an official release. The vaccine can be handle in an unfrozen, liquid formulation that can be stored at 2 degrees Celsius to 8 degrees Celsius, allowing for distribution using standard vaccine channels, it added. Early trial data published in The New England Journal of Medicine showed the vaccine appeared safe and also led to the production of high levels of virus-fighting antibodies in volunteers. It will, however, take months — probably early 2021 — before we know if the vaccine is successful, a report in the BBC said. Janssen-Johnson&Johnson vaccine: Known as Ad26.COV2-S, the vaccine is developed by Johnson & Johnson-owned Belgian company Janssen. This trojan virus vaccine uses a human adenovirus for its version and is the only option in the advanced US testing aiming to show if a single dose rather than two would be enough. According to a report on BBC.com, the NIHR Southampton Clinical Research Facility had last week started the recruitment of 6,000 volunteers for a trial. Another 30,000 volunteers from other countries are expected to join the phase three trials of the vaccine. The report said that the “Janssen-Johnson&Johnson vaccine uses a common cold virus that has been genetically modified to make it harmless and to look more like coronavirus at a molecular level. This should train the immune system to recognise and fight the coronavirus.” The UK government has ordered 30 million jabs of the Janssen-Johnson & Johnson vaccine. According to a report in The Economic Times, Johnson & Johnson has licensed the manufacturing of the vaccine to Hyderabad-based Biological E. The US drugmaker has transferred technology to Biological E and has given it manufacturing rights for its Covid-19 vaccine, which may become available in India by mid-2021.
The Chinese Four
China has been bullish about the development of its vaccine for the novel coronavirus with four vaccines now in late-stage testing. In fact, according to AFP, China has been giving experimental Covid-19 vaccines to people including state employees, international students and essential workers heading abroad since July. Many of the trials are taking place overseas, as China claims to have largely brought the virus under control within its borders. Some of the major vaccine candidates include two vaccines made by Sinopharm – the BBIBP-CorV and a similar Wuhan vaccine – the CanSino Vaccine and the Coronavac by Sinovac.
Sinopharm vaccines: Sinopharm is testing the two vaccines in late-stage trials in countries including the UAE, Bahrain, Egypt, Jordan, Peru and Argentina. The company claims to have inoculated one million people with its experimental vaccines. The company also claimed last week to be “leading the world in all aspects” of vaccine development, although it did not offer clinical evidence from ongoing trials. Instead, it cited anecdotal experiences from those who have been inoculated, including “construction personnel, diplomats, and overseas students” who it said have gone on to visit more than 150 countries after vaccination without being infected. One of China’s front-runner vaccine candidates, the BBIBP-CorV is a chemically inactivated whole vaccine virus developed by the Beijing Institute of Biological Products, a subsidiary of the state-owned China National Pharmaceutical Group Sinopharm and China National Biotec Group are all subsidiaries of the parent CNPG). Whereas the Wuhan vaccine candidate is similar to the BBIBP-CorV except that it is developed by the Wuhan Institute of Biological Products (a subsidiary of Sinopharm). CanSino vaccine: Developed by CanSino Biological Inc and Beijing Institute of Biotechnology, the Ad5-nCoV is another adenovirus-based vaccine similar to the Oxford vaccine, the Sputnik V, and the Janssen vaccine. Just like the Sputnik V in Russia, China’s government has authorised the emergency use of the CanSino’s adenovirus shots in the military ahead of any final testing. [caption id=“attachment_8922971” align=“alignnone” width=“640”] China is rapidly increasing the number of people receiving its experimental coronavirus vaccines, with a city offering one to the general public and a biotech company providing another free to students going abroad. AP[/caption] CoronaVac: Developed by China-based Sinovac Biotech, the CoronaVac is expected to reveal its interim results on its efficiency based on trials in Brazil by early December, reports said. According to BBC.com, a study involving 700 people showed the vaccine triggered a quick immune response, although the study conducted in April and May this year did not give a percentage of the vaccine’s success rate. According to the report, “Zhu Fengcai, one of the paper’s authors, said the results - which are based on 144 participants in the phase 1 trial and 600 in the phase 2 trial - meant the vaccine was ‘suitable for emergency use’”. According to AFP, the governor of Sao Paulo in Brazil has signed a deal with Sinovac to buy a total of 46 million doses – six million produced in China and the remainder produced in Sao Paulo – of the vaccine. However, Brazil’s president Jair Bolsenaro is against the deal. Earlier, Brazil’s national health regulator Anvisa had
suspended the trials of the vaccine in October after one of the recipients showed an adverse reaction to the vaccine. The Butantan biomedical research institute, which is conducting trials in Brazil, said Monday that it has gathered enough data to have interim results on its efficiency in early December. Sau Paulo received the first batch of 1.2 lakh vaccines on 19 November, according to
Reuters. The doses will be stored in an undisclosed warehouse as the state awaits approval for use in Brazil by Anvisa, which according to the latest reports is expected by the first week of January. Final Phase 3 trials to assess the efficacy and safety of the vaccine are still ongoing in Brazil, Indonesia, and Turkey.
India-based vaccine candidates
Covishield: As stated earlier, this vaccine candidate is developed at the SII’s Pune laboratory with a master seed from Oxford University/Astra Zeneca. The Covishield vaccine candidate is currently undergoing phase 2/3 clinical trial at 15 different centres across India, according to ICMR. It announced the completion of the enrolment process for phase three trials on 12 November. The vaccine made in the UK recently announced an efficacy of 70 percent following trials in the UK, Brazil, South Africa, and the US. It’s possible that following the foreign trials, the DCGI may approve the vaccine for emergency usage if gets a similar approval abroad. SII has already manufactured 40 million doses of the vaccine, under the at-risk manufacturing and stockpiling license from DCGI. [caption id=“attachment_8555391” align=“alignnone” width=“640”] An illustration of COVAXIN, the vaccine candidate for COVID-19 developed by Bharath Biotech. Image: Bharath Biotech[/caption] Covaxin: On 20 November, Bharat Biotech initiated the phase three efficacy trials of the COVAXIN, an indigenous vaccine candidate developed by Bharat Biotech in collaboration with ICMR’s National Institute of Virology in Pune. BJP leader and Haryana health minister Anil Vij was the “first volunteer” for the Phase-III clinical trial. He received the dose in Haryana. The company has also started phase III trials in Odisha. Overall, the Phase 3 trial of COVAXIN will involve 26,000 volunteers across 25 centres in India and is being conducted in partnership with the ICMR. It is the largest clinical trial conducted for a COVID-19 vaccine in India. The vaccine has successfully completed the interim analysis of Phase 1 and 2 trials. The human trial of Covaxin had begun at Rohtak’s Post Graduate Institute of Medical Sciences in July. Covovax: ICMR and SII have also collaborated for the clinical development of COVOVAX developed by Novavax and upscaled by SII. The Pune-based company has received the bulk vaccine and Matrix-M adjuvant from Novavax and will soon fill and finish them in vials. This Covovax will be tested in a Phase 3 trial in India and an application for the same to regulatory authorities will be made soon by ICMR and SII, the ICMR said in a recent release. ZyCov-D: According to reports, Ahmedabad-based Zydus Cadilla has completed phase two trials of the vaccine candidate in India and is awaiting results. According to a
report in Business Today, Zydus Cadilla is expecting to begin phase three trials of the vaccine candidate by December among 30,000 volunteers. According to PTI, those who were administered the vaccine in phase one trials, the company reported, found the vaccine “well-tolerated”. The ZyCov-D vaccine is a plasmid DNA vaccine. “In this, plasmid DNA, a small circular piece of DNA found in the cells, would be introduced into the host cells, where it would be translated into the viral protein and elicit a strong immune response in the human immune system,” the report said. The drug manufacture is reportedly also working on a live attenuated recombinant measles virus vectored vaccine against COVID-19. “The recombinant measles virus (rMV) produced by reverse genetics would express proteins of the novel coronavirus and will induce long-term specific neutralising antibodies, which will provide protection from the infection,” the report added. Biological E’s vaccine candidate: Besides manufacturing the Janssen-Johnson & Johnson vaccine**,** the Hyderabad-based Biological E Ltd is also working on another vaccine, which hopes to start production by summer 2021. The company began adaptive Phase I and II human trials for its COVID-19 vaccine candidate after getting approval from DCGI. It expects to get the results back by February, next year. According to the
press release, the trial will test two doses of the vaccine in around 360 volunteers who are aged between 18 to 65 years, injected 28 days apart. The vaccine will include an antigen from Baylor College of Medicine (BCM ventures) in Houston, Texas, and Dynavax Technologies Corp’s advanced adjuvant CpG 1018. An adjuvant is a substance that increases the potency and regulates the immune responses to an antigen to improve it. [caption id=“attachment_9004101” align=“alignnone” width=“640”]
 Representational image. AP[/caption] According to a
report in Economic Times, the company is also hoping to begin phase three trials by January-end and begin producing the vaccine by summer. Biological E’s MD Mahima Datla told the newspaper that the company is currently evaluating four different formulations depending on different antigen strengths in the phase I-II combined studies. Based on the preliminary immunogenicity data from 400 people in phase one and phase two trials, which is expected by end of January, the vaccine candidate will enter into phase-III trials. About 30,000 people are expected to participate in the final phase trials, the report said. Indian Immunologicals: Also based in Hyderabad, the Indian Immunologicals is reportedly in talks with Moderna to manufacture the mRNA vaccine in India.
The exception: Mynvax’s warm vaccine
An IISC Bangalore incubated startup, Mynvax has developed a vaccine candidate by reverse-engineering the Receptor Binding Domain (RBD) of the Spike Glycoprotein found on the surface of the SARS-CoV-2. Mynvx co-founder and professor at IISC Professor at IISc’s Molecular Biophysics Unit Dr Raghavan Varadarajan told YouStory.com during an interview that early phase animal trials showed that the antibodies elicited could neutralise the replicating novel coronavirus even in high dilution. According to a Deccan Herald report, the company hopes to complete the animal trials by December, and then move to process development, animal safety and toxicity studies, and, then clinical trials. If found effective, the vaccine could be a major breakthrough for India, as it has been found to be stored at 37 degrees Celsius, thus making it an ideal candidate for distribution in a country like India which lacks sufficient cold chain facilities. The startup is currently trying to secure sufficient funding to enter clinical trials. “Rs 15 crore is required for the vaccine to be administered in human clinical trials. If everything goes well, the vaccine can be licensed by mid-2022,” The Deccan Herald report quoted Varadarajan as saying.
NO permanent cure yet
While the efficacy results of the four major contenders are promising, and several other vaccine candidates have shown positive results in the early phase trials, Harvard immunologist Michael Mina told AFP that several important questions related to COVID-19 vaccine candidates remain to be answered. The most important of them all being the duration of protection. When the vaccines are first administered, immune cells secrete huge numbers of antibodies, but these are temporary, and “all of the efficacy data that we have gotten from the vaccine recipients is generally within just a few months,” he said. We don’t yet know whether, after around six months, the immune system’s “memory cells” will be activated to make new antibodies if it encounters the virus again. We also don’t yet have detailed data on how either vaccine works on the elderly, who have weaker immune systems and are the most vulnerable to COVID-19. And finally, another open question is whether the vaccines stop people who are exposed to the virus from transmitting it to other people, even though they may be themselves protected from the disease. Nevertheless, Weissman is upbeat about the platform’s future potential, noting that development is already underway for herpes, influenza, and HIV vaccines. There is also the question about the effects that the vaccines might have on effects on different age groups such as people with comorbidities which needs to be studied. With inputs from agencies


)

)
)
)
)
)
)
)
)



