The growing population and ascend in chronic care needs are wielding substantial demands on our healthcare frameworks. It is greatly stressing that about 50-60 million Indians are constrained to spend half of their yearly family income to address medical issues, particularly with regards to hospitalisation. The out-of-pocket costs for medical services are extremely high for us, which influence disservice to almost 7 percent of our population. Access to capital has been one of the biggest roadblocks to the growth of the Indian healthcare sector. Today, majority of the system constitutes of private healthcare and the Indian government spends only about 1 percent of its GDP on healthcare, which is among the lowest globally for any country. However, to meet India’s burgeoning healthcare needs, both the public and private sector will have to join hands to build value-based and cashless healthcare. This implies providing a high-end care at a subsidised cost compared to other countries; to enhance healthcare services. It is the commitment of the state to give free and universal access to quality healthcare services to its citizens as India keeps on being among the nations of the world that has a high weight of ailments. The various well-being projects and policies in the past have not possessed the capacity to accomplish the coveted objectives and targets. However, the recent launch of one of the major policy initiatives by the government, Ayushman Bharat – National Health Protection Mission for the underprivileged section of Indian population, will help in the accomplishment of the dream of Universal Health Coverage of the Indian population. Ayushman Bharat is an attempt to ensure that universal healthcare reaches the weaker section of the society and it may certainly boost the ratio of people availing primary healthcare and some of the secondary healthcare. But the current framework of the scheme will not be beneficial for people who need tertiary care as the remunerations under the scheme will not be sufficient to avail value based healthcare.
Under the scheme, tertiary healthcare service providers will be forced to cut costs at every level which will lead to offering a sub-standard healthcare to patients under the scheme. They may not be able to avail the necessary medication, technology and clinical expertise to get the best outcome and will soon lose confidence in the system.
However, implementation of the scheme will be a big challenge since it would involve focusing on the critical success factors, maintaining good quality of care for patients, strengthening primary care and healthcare infrastructure. Quality of patient care A scheme of such scale is most likely to face obstacles when ‘quality of patient care’ is considered. In case of serious and major illness, emergency and ICU care, there is a high chance of an Ayushman patient to receive low quality healthcare due to the capped amount to be granted. Hence, the mortality and morbidity rate will be very high. [caption id=“attachment_5280511” align=“alignleft” width=“380”] 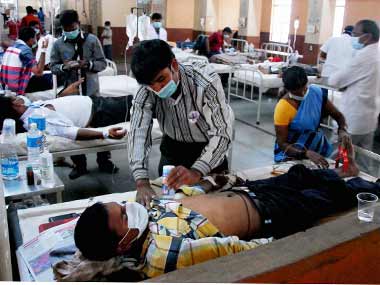 Representational image. PTI[/caption] The trust and confidence of the poor will be immensely affected. Let’s say, if I am a below poverty line (BPL)person and I require a certain drug treatment for my cure, if the system doesn’t pay, I’m helpless. So, I will not get the right treatment and survival is at stake. Therefore, if you are an Ayushman patient you will get low quality care as the amount paid is less compared to the cost of the treatment. For the vulnerable class, the government funding is essential to make healthcare universally available but there is also a need to improve the outcomes for the money spent- only then we can make value-based healthcare a reality. Strengthening primary care and healthcare infrastructure Giving financial protection to the poor not only gives them access to healthcare but is also cost-effective. That is, it gives great incentives as the advantages of financial protection far exceed the expenses. However, cost-effective health coverage must cover primary care. The WHO prescribes allotment to primary care, particularly for presently unprivileged low-income population. In India, reallocation of assets is important to fortify primary care and to embrace innovation and well-being programs, to be cost-effective in terms of expenses and anticipated benefits. Solid primary care is crucial to keeping overall access to healthcare reasonable and inexpensive in the nation. Our greatest imperative to getting this going isn’t lack of capital or framework, but an intense deficiency of human resources and infrastructure. Most public healthcare facilities have noteworthy deficiency of specialists, doctors, nurses and other healthcare experts. To address this, the government should use existing foundation in private medical schools, that has been under-used because individuals can’t afford the cost of it. To utilize these spaces, bundle rates must be made competitive and at standard with the market rates. The government says that volumes will help take care of the expenses, yet that is after a point of time. Now, they must get the beneficiaries, and make it reasonable for the hospitals as well. Outcome based payments Quality Healthcare is defined as value-based medicine that is assessed by outcome. Today, nearly 80 percent of healthcare in India is provided by the private healthcare system and in order to meet the burgeoning healthcare needs of Indian population through value based medicine, the country needs a synchronised effort by both private and public sector. The scheme encourages hospitals to maintain certain minimum standards. The reward to hospitals is 10 percent higher if they have National Accreditation Board for Hospitals and Healthcare Providers (NABH) accreditation and a basic technology criterion has been stated for hospitals to be qualified for this scheme. Hospitals that meet certain quality benchmarks ought to be permitted to serve NHPS beneficiaries. Quality should be assessed not only by the infrastructure offered at the hospital but also by authentic patient outcomes attained.
The only solution is to have a mandatory universal health cover for all sections of the society.
This will increase the pool and allow cross-subsidy between the government and the private sector for different sections of the society. Over and above, the power to judge the need should be with an autonomous insurance company that can negotiate with the private service providers on a reasonable remuneration which is beneficial for both parties. It is a proven and successful model followed by various developed countries and will bring a sustenance in India as well. It is a long road to make quality healthcare accessible but we need to take up the challenge and pave way for a correct system where people receive right treatment at the right time irrespective of their economic status. Over the long haul, Ayushman Bharat should focus on fortifying of primary care, incorporation of outpatient treatment and general health care delivery framework with a specific end goal to make government’s progress to accomplish Universal Health Coverage. (The writer is a doctor and Chairman & CEO, Health Care Global Enterprises Ltd.)


)

)
)
)
)
)
)
)
)



