The dangerous country-wide stock-out of second-line and paediatric drugs in treating tuberculosis is yet another example of the hidden risks of centrally controlled vertical programmes in a complex country such as India. This shortage can lead to a disastrous situation in which the government causes more harm than benefit: Many TB-patients, including children, can develop a stubborn drug-resistant TB, and an incurable “extensively drug resistant TB (XDR-TB)” because the government of India messed up. [caption id=“attachment_891525” align=“alignleft” width=“380”] 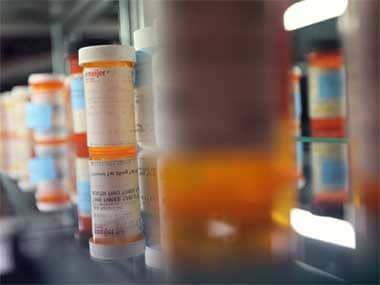 Public health activists say that paediatric drugs have completely run out, which means children with TB are facing treatment interruption. Getty Image.[/caption] Centralised procurement for national programmes, in which the Centre buys drugs for all the states, certainly has the advantage of economy-of-scale and ensuring uniform quality controls. However, in a paralysed government with defunct systems, it can also be a recipe for disaster as the current impasse shows. The Hindu reported on January 18 that “there is a massive stock-out of anti-TB drugs across the nation”. It also said that in every state, availability of first line drugs such as Rifampicin and Isoniazid will exhaust by the end of July. Public health activists say that paediatric drugs have completely run out, which means children with TB are facing treatment interruption. In the case of drug-resistance TB, drugs such as Capremycin, Ethionamide, PAS, cycloserine and INH are in short supply. Non-availability of drugs for TB are extremely alarming because patients need to take these drugs on time without fail till they are cured of the disease. Any interruption can lead to the disease-causing bacterium developing resistance and the disease becoming untreatable. In fact, a major problem with India’s TB-burden is the load of drug-resistant TB. In most cases, the patient becomes drug-resistant because of incomplete or irregular treatment. The patients can transmit their drug-resistant illness to others, who will be saddled with an infection that is hard to treat. A large number of them will die; those who survive will have to undergo treatment that is expensive and toxic. Once a patient develops drug resistance, it is a tragedy for three reasons: One, the second line drugs are not as effective as the first line and takes at least three times longer if at all they work; two, the drugs are toxic; and three, they are far more expensive. If the first line and second line drugs don’t work, the patients get into an utterly dangerous zone of XDR-TB which is more or less untreatable. The so-called third line is not of reliable efficacy. In view of an immense challenge posed by MDR-TB, the US FDA had recently given an early approval to a drug called Bedaquiline and the WHO even made an unprecedented step of making interim recommendations based on Phase II B clinical trial data. This was the first TB drug to be invented in the last 50 years. The critical point in TB treatment is adherence - right time and right dosage without fail. Failure in adherence will not only fail to cure the disease, but will also lead to drug resistance. This is exactly what the present stock-out threatens. And to learn that it was caused by a national government is certainly startling. It’s criminal neglect. Reportedly, the present stock-out is because the health ministry failed to buy the drugs on time. Besides failing in timely tender processes, it advised the states only at the last minute that there could be shortages in supply. The states, however, had been dependent on the Centre, through the Revised National Tuberculosis Control Programme (RNTCP), and hadn’t anticipated such a crisis; hence they couldn’t make alternative arrangements. There were exceptions such as Tamil Nadu, which traditionally has a very strong public health infrastructure, including an efficient drug procurement and distribution system. States with poor resources - money, technical and personnel - will suffer. As MSF noted, “the stock out is related to the never-ending issues with drug procurement that India faces in many of its public health programmes - the routine but deadly delay in tendering for these drugs - and the resulting drug stock outs are one of the reasons why India has one of the world’s highest burdens of DR-TB.” Now the moot question. Why should the government of India run such massive and messy vertical health programmes when health is a state subject? These top-down initiatives fail to see the socio-economic diversity of the states and hence roll out uniform programmes irrespective of the track-record of the state governments. While they may bring relief to badly governed states, in states which are in better shape, these national programmes steamroll existing and well-running local initiatives. Once the national programmes take control, the states have no roll but to fall in line and implement. Given the suspect efficiency of the central ministries and lack of political will (health is one of the least glamorous ministries), shortage or interrupted supply of drugs and delayed delivery of funds and equipment are routine. As the TB drug stock-out shows, they can also make the situation worse. Another big vertical programme run by the Government of India is on AIDS. It does have a decentralised network all the way to the districts, but because its nervous system is in Delhi, shortage of ARV drugs, blood-safety implements and funds for NGOs have been routinely reported. It’s hight time that the Government of India restricted itself to advising the states and providing them with policy advice, technical and financial support. Although pooled procurement has its benefits, it should not go beyond negotiating on behalf of the states. The Centre should stop implementing public health programmes and instead should empower the states to do that. Instead of wasting money, it should contribute to the states’ plan expenditure. Trying to manage the health of people, which should happen at local levels, from Delhi is not only foolish, but also is fraught with danger and wastage of resources. This crisis is just one of the many examples.
Once a patient develops drug resistance, it is a tragedy for three reasons: One, the second line drugs are not as effective as the first line and takes at least three times longer if at all they work; two, the drugs are toxic; and three, they are far more expensive.
Advertisement
End of Article


)
)
)
)
)
)
)
)
)



